Header logo
header top contact widget
Blog Archives
Recent Posts
Categories
Archives
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- August 2014
- July 2014
- June 2014
- May 2014
- April 2014
- March 2014
- February 2014
- January 2014
- December 2013
- November 2013
- October 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- April 2013
- March 2013
- February 2013
- January 2013
- December 2012
- November 2012
- October 2012
- September 2012
- August 2012
- July 2012
- June 2012
Think ‘Vaping’ Is Safer For Smile Than Cigarettes?
Posted on Jan 28, 2016 by William J. Claiborne, DDS MS
The popularity of ‘vaping,’ particularly with younger E-cigarette smokers, has sparked a growing health concern since hitting the market in 2004. This concern has motivated the National Institute of Dental and Craniofacial Research to implement a study on the effects of vaping’s aerosol mix to tissues in the mouth, lungs and airway structures.
The study, slated to begin in February 2016, will not focus on the effects of nicotine but of the impact of vaporized chemical delivery to tissues. Studying the effects of long-term chemical exposure to tissues through this means will hopefully provide a more accurate assessment of their safety.
Unlike traditional cigarettes, E-cigarettes use a moist vapor to deliver a mix of nicotine, formaldehyde and other chemicals. Because oral tissues are moist by nature, the water vapor that is inhaled is readily absorbed by soft tissues in the mouth.
Prior research has shown that nicotine is harmful to oral health, regardless of how it arrives — cigarettes, snuff, chew and now vaping. Nicotine is known to have a drying effect on oral tissues, which decreases saliva that helps rid food particles and bacteria from the mouth. When drying agents deplete saliva, oral bacteria reproduce more rapidly. This increases the risk for tooth decay and periodontal (gum) disease.
Because nicotine also constricts blood vessels in the mouth, it compromises the ability of oral tissues to heal. This is why we advise patients to stop smoking following extractions or implant placement so healing is not slowed. ‘Vapers’ should also be concerned about the bad breath associated with dry mouth, if nothing else.
The misconceptions about vaping’s safety may be to the detriment of your smile. Hopefully, the findings of this research will reveal the true level of risk so users can adjust their oral care commitment accordingly.
In the meantime, if you smoke, vape, chew or dip, pay particular attention to your oral health. Be especially committed to your oral hygiene at home as well as your 6-month dental check-ups. These visits can help you maintain a healthy mouth and avoid problems – or catch those that occur at their earliest stages.
If you feel your oral health has been neglected or compromised due to smoking, chewing, or vaping, call 828-274-9440 to schedule an appointment. And relax, we’re a ‘lecture-free’ zone!
Post-Menopausal Women At Higher Risk For Gum Disease
Posted on Jan 26, 2016 by William J. Claiborne, DDS MS
Menopause is typically accompanied by hot flashes, night sweats, fatigue and moodiness. Once a female enters the post-menopausal phase, these symptoms may subside while a new problem emerges. Research has shown that being post-menopausal heightens the risk of tooth loss.
Studies have revealed that bone loss in postmenopausal women can be accompanied by a greater risk for periodontal (gum) disease. A study published by the National Institutes of Health cited that post-menopausal females with signs of osteoporosis had an increased liklihood of gum disease when compared to post-menopausal women with no signs of osteoporosis.
It has long been known that a reduction in estrogen levels contributes to bone loss. Post-menopausal women may also experience a reduction of saliva, which increases the potential for cavities.
The estrogen drops of menopause also increase the risk for heart disease and Alzheimer’s disease. While hormone replacement therapy (HRT) can alleviate symptoms associated with estrogen deficiency, replacing estrogen may also prevent some of the chronic illnesses common to postmenopausal women.
Our goal is to provide care to each patient that takes their overall health into consideration. This is why we ask you to keep your health history and medication list up to date. This information enables us to customize your care to your unique needs. This can also help you avoid problems or minimize those that do emerge.
If you are post-menopausal, be especially aware of the signs of gum disease. These include gums that bleed when brushing, sore or tender gums, receded gums that expose darker tooth root sections, gums that darken in color, persistent bad breath or pus pockets that form at the base of some teeth. Call 828-274-9440 to schedule an examination at your earliest convenience.
Bad Breath Origins & How To Keep It At Bay
Posted on Jan 20, 2016 by William J. Claiborne, DDS MS
If you wonder, “Do I have bad breath?” you probably do.
Occasional bad breath, though unwanted, is not unusual. After morning cups of coffee or an onion-laden meal, we can all emit less-than-welcome odors. Unfortunately, bad breath can have a lasting impression, a negative one. Frequent bad breath can even cause others to avoid close encounters as they anticipate having to inhale an offensive odor.
Bad breath can be the result of several problems. Some health problems can contribute to bad breath, including acid reflux and illnesses such as sinus infections, bronchitis and liver problems.
However, the most common cause of bad breath is the result of accumulated oral bacteria. Bacteria are living organisms that eat, reproduce and emit waste on a continual basis. Inadequate oral hygiene enables oral bacteria to develop into bad breath.
Without regular brushing and flossing, oral bacteria reproduce and plaque forms. Plaque is the sticky film you feel on teeth. When not removed, plaque hardens into a substance known as calculus. This is an accumulated colony of oral bacteria that attaches to tooth surfaces and dines on tooth enamel and gum tissue.
Sugary drinks and foods high in carbohydrates are the ideal food for oral bacteria. Consumption of these enable bacteria to reproduce more rapidly, accelerating their ability to grow and thrive in your mouth.
Persistent bad breath is also a symptom of gum disease. Other signs are gums that are tender and bleed when brushing. The color of your gum tissues may also seem darker in color than a healthy pink.
If signs of gum disease are present, there are various treatments that can restore your mouth to a healthy state depending on the level of gum disease present. As with anything, the earlier you have treatment, the less involved the process will be. Early treatment can mean a significant savings in treatment time and money.
If gum disease is not the source of your breath odor, another reason could be ‘dry mouth.’ Dry mouth causes your mouth to become stale and sticky. An example of dry mouth is when you first wake up. Since saliva flow is reduced during sleep, oral bacteria are not removed efficiently. This causes oral tissues to dry out and allows bacteria to accumulate.
The tendency to snore or breath through the mouth are habits that also contribute to dry mouth. If you smoke, dry mouth is a common side effect. Cigarette smoke contains chemicals that are severely drying to oral tissues. Alcoholic beverages are drying, as well, as is coffee. Some medications also have side effects that include oral dryness.
When you examine the true origin of most bad breath, oral bacteria is at the root of the problem in the majority of cases. To avoid (or greatly minimize) bad breath, begin with a clean, healthy mouth. If you haven’t had regular dental check-ups and cleanings, see a periodontal specialist to help you establish a foundation of good oral health. A Periodontist is a dental specialist who has advanced training in the treatment of gum tissues in the mouth. He or she is your best choice for establishing a mouth with minimal bacteria influences.
Once your oral health is in good shape, it’ll be easy to keep it there with the following steps:
– Brush at least twice daily for at least two minutes each time. Finish up by brushing your tongue to loosen embedded bacteria there, including the back of the tongue.
– Floss daily. If this is difficult, invest in an electronic flosser.
– Keep your mouth moist by drinking lots of water. If you take medications that have dying side effects, ask about oral rinses that can help to boost saliva flow.
Why worry about your breath when you can speak, laugh, whisper and kiss with confidence! Call 828-274-9440 and begin with a no-cost consultation. During this time, we’ll discuss your current oral health and how to achieve a healthy mouth and fresh breath.
How Gum Disease Forms – Dental Terms Made Easy
Posted on Jan 15, 2016 by William J. Claiborne, DDS MS
A friend who recently acquired a sail boat loves to talk about his new passion. Unfortunately, as he casually throws out terms such as halyard, fife rail, and jibe when describing his outings, I become “lost at sea” (pun intended!). Rather than stop his conversation at each unfamiliar term for an explanation, I tend to try to absorb what I can. More than not, I fail to truly grasp the actual picture of what he is sharing.
As a Periodontal Specialist, I have to continually remind myself that some dental terminology that’s second nature to me isn’t as clear to the patients with whom I’m communicating. Just as jibe means very little to me, terms like osseointegration and mandibular are not familiar ones, often leaving the patient drifting as the conversation begins to fall apart.
Although dental implant placement and gum recontouring are regular treatments our office provides, gum disease is the most frequent problem we treat. Gum disease in the U.S. affects over 70% of adults at some level. It is the leading cause of tooth loss and has been linked to heart disease, high blood pressure, stroke, memory loss, arthritis, diabetes, preterm babies and impotency.
Because gum disease (also known as periodontal disease), begins without obvious symptoms, people often ignore the warning signs, which merely allows the disease to progress further. In order to help people have a clear, concise picture of how gum disease forms, I’ve broken the stages down in language that removes dental jargon.
• Oral bacteria – We all have bacteria in our mouths. That’s normal. However, it’s the excess of bacteria that is at the root of the problem. When oral bacteria are not brushed, flossed or rinsed from the mouth properly and on a daily basis, they band together and form plaque.
• Plaque – This is a sticky film that coats teeth. It also covers the gums and tongue but is not as obvious as what can be felt by running the tongue over teeth. The presence of plaque means the mouth contains more bacteria than saliva flow can handle. When plaque is not removed, oral bacteria continue to reproduce, thrive and form calculus.
• Calculus – Also known as tartar, this is actually a hardened form of bacteria that emerges from plaque. As a condensed colony of bacteria, calculus attaches to teeth and can only be removed with special instruments used by dental professionals. This is why your 6-month check-ups and cleanings are so important. By scraping away buildup on a regular basis, you can halt damage to gums and enamel.
• Gingivitis – This is actually the first stage of gum disease. In this stage, oral bacteria are attacking gum tissues and tooth enamel as they reproduce at a rapid rate. Signs of gingivitis are gums that bleed when brushing, sore spots and frequent bad breath. It is this stage, however, that can be self-treated. That is to say that an immediate response with proper measures can combat the problem before it worsens. This includes a minimum of twice daily brushing (at least two minutes each time) with a soft to medium bristle tooth brush and flouridated tooth paste. Daily flossing is also needed to remove food particles and bacteria between teeth. Tongue scraping is advised, also. This removes oral bacteria that is embedded in the grooves of the tongue. When a tongue scraper is not available, brush the tongue with your tooth brush after brushing teeth. Be sure to get to the back of the tongue where the greatest concentration of bacteria live. Drink lots of water and swish daily with an oral rinse that kills bacteria and provides added protection to enamel.
• Periodontal (Gum) Disease – When gingivitis is not resolved, the next stage you can expect will be periodontal disease. This is when the bacteria have moved down into the gum tissues and are eating away at gums and tooth enamel at a rigorous rate. Typical symptoms are red and swollen gums, gums that bleed easily when brushing, 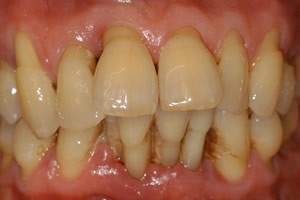 gums that pull away or loosen from teeth, exposing sensitive tooth root areas. Persistent bad breath is another symptom, which occurs even after brushing or chewing gum.
gums that pull away or loosen from teeth, exposing sensitive tooth root areas. Persistent bad breath is another symptom, which occurs even after brushing or chewing gum.
• Periodontitis – At this stage, gum disease is running rampant in your mouth. Gums are red and tender all the time. Pus pockets form at the base of some teeth. Some teeth will begin to loosen as bacteria eat away at the structures that support tooth roots. Eventually, some (or all) of your natural teeth will need to be removed.
I believe if the general population were more aware of the sequence that leads to full-blown gum disease, we’d have far less adults walking around with bacteria that causes internal inflammation. When oral bacteria enter the bloodstream through tears in diseased gum tissue, it can trigger inflammatory reactions that are the foundation of the severe health problems mentioned prior (heart disease, arthritis, etc.). We’d also have fewer adults dealing with the ordeals surrounding tooth loss.
I hope I’ve provided a helpful explanation of how oral bacteria progresses and how it effects your oral and overall health. For an examination to determine the health of your gums, along with recommended treatment options, call 828-274-9440 to request an appointment.
Remember, if you are having any symptoms, these will only worsen when treatment is delayed. This typically means more treatment time and greater expense.


