Header logo
header top contact widget
Pregnancy Gingivitis
Females & Males – Oral Health Differences
Posted on Jun 05, 2024 by William J. Claiborne, DDS MS
As a periodontist, I have an intense understanding of how oral health impacts the overall health of both males and females. However, my specialized skills also allow me to understand the unique factors that affect the oral health of our female patients.
As a result of hormonal fluctuations, females can face particular challenges when it comes to oral wellness. For example, pregnancy gingivitis is not uncommon in women during pregnancy. If not treated and resolved, however, it can develop into periodontitis (advanced periodontal disease) and subsequent tooth loss.
A good illustration of how women face unique oral health challenges was noted in findings shared recently on Fox News. (https://www.foxnews.com/health/women-experience-dental-health-issues-men-experts-say-heres-what-do-about)
Using a pH meter, the pH levels in saliva were tested on multiple people over the course of many years. The researchers found the pH of women’s saliva was frequently 5.5 or 6 – a lower saliva flow rate than men.
Saliva’s ideal pH rate is between 7 and 7.4. If the pH of saliva constantly drops below 5.5, the tooth enamel gets demineralized, which means it will be more prone to tooth decay. Because the aging process causes a lower flow of saliva, a drier mouth weakens teeth due to the slower remineralization or buffering capacity.
Below are some of the different phases of life that can be accompanied by various challenges to a female’s oral health:
Puberty: Estrogen and progesterone hormones produced during puberty increase blood flow to the gums. This changes how the gums respond to plaque, the sticky film of bacteria in the mouth. With this may be gums that bleed when brushing and become red, tender, and swollen.
Menstruation: The menstrual cycle causes hormonal changes that cause some women to experience symptoms such as swollen gums that turn bright red, canker sores, or gums that bleed easily. Referred to as menstruation gingivitis, this usually occurs just prior to the onset of the period and resolves in a day or so.
Oral Contraceptives: Taking birth control pills that contain progesterone cause some women to have gum tissue inflammation. This occurs from heightened sensitivity to the toxins produced from the overload of bacteria that form plaque. While many women have less gum reactions after the first few months, some medications can lower the effectiveness of oral contraceptives. This reinforces the need to keep your dentist updated on all medicines you take.
Pregnancy: With each trimester of pregnancy, hormonal levels can change. Pregnancy also causes increased progesterone levels, which can increase the risk for plaque formation. This can lead to pregnancy gingivitis, particularly during the second to eighth month of pregnancy. This condition causes the gum tissues to become swollen and bleed easily. Gingivitis is the first stage of gum disease, which is why it is important to have gingivitis fully resolved to prevent its further progress. Because studies have found that gum disease can increase the risk for preterm and low birth weight babies, obstetricians are urging their pregnant patients to be particularly diligent in maintaining good oral health.
Menopause: With age, a variety of changes can take place in our mouths for both males and females. A particular challenge is the decrease in saliva flow, leaving the mouth is less moist. Additionally, the side effects of certain medications can pose challenges to keeping the gums healthy. Without adequate saliva flow to keep the mouth cleansed and efficient in neutralizing the acids from plaque, the risk for gum disease is greater for females in menopausal years. Declining estrogen levels also place women at greater risk for bone loss or osteoporosis as well as inflamed gum tissues around the teeth (called periodontitis). When there is bone loss of the jaw, it can result in tooth loss. Receding gums are a sign of this bone loss since more of the tooth surface is expose to the causes of tooth decay.
Researchers in Romania studied the gender differences in oral health. Through an online survey of 600 adults, the study assessed attitudes, behaviors, and educational understanding related to oral health and dental services.
The results show that women have more positive attitudes towards dental services with higher oral health values, better self-care behaviors, and have higher oral health literacy than men.
While the study indicated that oral care attitudes and behaviors of men had different influencing factors, women were primarily influenced by their level of oral health literacy. The study also noted that differences in oral health attitudes and values for both genders can be based upon education.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9604615/
This is a good reason to stay on top of how intricately your oral health is to your overall health. Because the bacteria of periodontitis can penetrate the bloodstream through weak gum tissues, it has been correlated to a long list of serious health problems.
Research has found that periodontal bacteria can trigger the development or worsen the likelihood of heart disease, stroke, some cancers (including pancreatic and lung
cancer), preterm babies, diabetes, arthritis, erectile dysfunction, Alzheimer’s disease and more.
Although gum disease can exist without obvious signs or symptoms, the most commonly noticed are:
• Red, swollen or tender gums
• Seeing blood in the sink when brushing
• Receded gums
• Loose or separating teeth
• Pus pockets on gum tissues
• Sores in the mouth
• Persistent bad breath
In our Asheville periodontal dental office, patients can begin with a private consultation. We are always happy to discuss oral health options with new patients. A referral is not needed.
Call 828-274-9440 to schedule.
Healthy Gums Advantageous To A Healthier YOU!
Posted on Apr 22, 2024 by William J. Claiborne, DDS MS
Periodontal (gum) disease and subsequent tooth loss has damaging effects to an individual, far beyond the mouth. When this was suspected decades ago, it prompted national agencies to track the oral health of the U.S. population. Using this extensive data, studies have revealed some interesting statistics, including how various age groups fare when it comes to oral wellness.
The following is mostly information pulled from the National Institutes of Health’s (NIH) “Oral Health In America” report. Released in December 2021, the findings were the culmination of years of research assembled by more than 400 contributors.
On a positive note, the percentage of Americans who have experienced tooth loss has declined since the 1970’s. As of 2016, complete tooth loss has fallen by more than 75% for adults between the ages of 65 – 75 years. Unfortunately, there is not good news when it comes to tooth decay – for nearly any adult age group.
For adults between the ages of 20 – 64, cavities have affected 90% and gum disease exists for nearly 50% of adults aged 45 – 64 years. This should be a concern for every American. This is because research has determined that the bacteria of periodontitis (advanced gum disease) can trigger or worsen a long list of serious health problems.
The list includes:
• Stroke
• Coronary Artery Disease
• Arthritis
• Diabetes
• Preterm & low birth weight babies
• Some Cancers (including oral and pancreatic)
• Alzheimer’s disease
• Impotency, Erectile Dysfunction (ED)
• Prostatitis (elevated PSA levels)
In addition to poor oral hygiene routines at home and avoiding regular dental cleanings and exams, high-risk behaviors (such as use of tobacco, opioids, and alcohol) accentuate the risks of gum disease.
Although gum disease can begin without obvious signs or symptoms, the most commonly noticed are:
• Red, swollen or tender gums
• Seeing blood in the sink when brushing
• Receded gums
• Loose or separating teeth
• Pus pockets on gum tissues
• Sores in the mouth
• Persistent bad breath
While the report found that there are stark differences in adult groups who had less access to having regular oral health care, disparities also stem from underlying economic, demographic, and societal inequities.
Below are some of the oral health variations pertaining to certain groups.
ADOLESCENTS
During the past 20 years, the percentage of adolescents (ages 12 − 19) having at least one molar with a sealant applied has nearly tripled, from 18% to 48%. That’s a good thing. Even so, there has been no decline in untreated tooth decay in adolescents since the last surgeon general’s report twenty years ago.
High caries (cavities in teeth) experienced in early childhood is the strongest indicator of caries problems that will be experienced in adolescence and adulthood. This means that when the factors contributing to developing cavities in childhood persist, the incidence of caries affecting permanent teeth will continue to increase during adolescence. Likewise, misalignment of teeth that exist or develop during adolescence can substantially impact eating, speech, gum health, and even psycho-social development. (Imagine a teen with teeth so mispositioned that they are ridiculed by peers.)
OLDER AMERICANS
There is good news for our older population (Americans over the age of 65). Their overall oral health has significantly improved over the past two decades with fewer teeth being extracted. Additionally, the proportion of the population with edentulism (no remaining natural teeth) is at an all-time low.
The not-so-great news… tooth loss remains a problem for older adults. Today, 1 in 6 Americans have no remaining natural teeth. At this rate, by the year 2030 (just 6 years from now), the 65-&-over age group without teeth will increase to 1 in 5.
For adults over the age of 75, the challenges are even greater. Over 54% have fewer than 21 remaining teeth with the number increasing to 80% for those living in poverty. With age also comes the increased prevalence of systemic diseases that may impact the mouth, making older adults more susceptible to oral health issues. (This includes heart disease, diabetes, arthritis, etc.)
Fortunately, things are moving in a positive direction for older adults, with more keeping their teeth than any previous generation. This has largely been the result of having increased attention on the benefits of prevention and improvements in treatments for gum disease and cavities, along with a decrease in the rate of smoking. (About 8 of every 100 adults – 8.3% – of adults 65 years and older were reported to smoke in 2023.)
WOMEN
Women have unique oral health concerns due to changing hormone levels based on menstrual cycles, pregnancy, and menopause. These fluctuations can raise the risk of oral problems that effect teeth or gums. Health issues, such as diabetes, can also affect the oral health of females.
To keep your teeth healthy, it is important to remove dental plaque. This is a sticky, colorless film of bacteria that coats teeth and gums. Plaque buildup can cause tooth decay and gum disease.
Even teeth that already have fillings are at risk for tooth decay. Plaque can build up underneath a chipped filling and cause new decay. And if there are areas in your mouth where your gums have pulled away from the teeth (known as receded gums or gum recession), the exposed tooth roots can decay as well.
It’s important – for all ages – to be committed to their oral hygiene time at the sink, at least twice a day. Devoting these minutes to the care of your teeth and gums will pay off in future years, helping to minimize costs for dental repairs and time in treatment. And, when early ages get into the habit of an oral care routine at home, they are more likely to carry that into adulthood.
Here are some easy brushing tips:
• Use fluoride toothpaste, which is an ingredient of many products. Fluoride protects teeth from cavities, helping to strengthen the tooth’s hard outer surface – the enamel.
• Angle the bristles toward the gumline so they can sweep away bacteria between the gums and teeth.
• Brush gently using small, circular motions. Do not scrub hard back and forth, which can wear down tender gum tissues and wear away tooth enamel.
• Brush all sides of each tooth and the tops (where debris and bacteria can hide within grooves).
• Brush your tongue, especially towards the back where the majority of bacteria embed. Swish well with water at least twice afterwards.
Cleaning between teeth to remove plaque is also part of a good oral hygiene routine. If plaque is not removed, some of it can harden below the gum line and irritate the gums. The gums become red, swollen, and may bleed easily. These are signs of gingivitis. Gingivitis caused by plaque buildup is a mild form of gum disease, and you can usually reverse it with daily brushing and flossing.
If plaque stays on your teeth for too long, it can harden. This hardened plaque is called calculus, or tartar. The only way to remove tartar is to have your teeth cleaned by a dentist or dental hygienist. If the tartar is not removed, the gingivitis can get worse and lead to more severe gum (periodontal) disease. In advanced stages, gum disease causes sore, bleeding gums; painful chewing problems; loose teeth; and even tooth loss.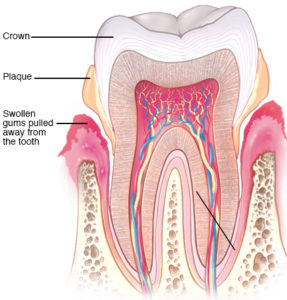
Here are some additional ways to keep a healthy smile with practical measures.
- Floss to remove plaque, and food particles, from between your teeth.
- Visit the dentist for routine check-ups and professional cleaning. If you are at a high risk for tooth decay (for example, if you have a dry mouth because of medicines you take), your dentist or dental hygienist may give you a fluoride treatment, such as a varnish or foam during the office visit.
- Drink fluoridated water. Drinking water with the right amount of fluoride protects your teeth throughout the day.
- Don’t smoke. Smoking increases your chance of gum disease. If you smoke and want to quit, there are many resources to help you: FDA’s Center for Tobacco Products, CDC’s Quit Smoking website, and the BeTobaccoFree.gov website.
- If you are planning to become pregnant, have a dental checkup. Because of hormonal changes, pregnant women may develop gingivitis and experience gums that are swollen and bleed easily. During pregnancy, it is especially important to practice good oral hygiene to maintain the health of your gums.
- Eat a diet that is low in sweets and sugary drinks.
A periodontal specialist is your best advocate in restoring or maintaining healthy gums. In addition to the skills in treating all stages of gum disease (from gingivitis to periodontitis), a periodontist specializes in the selection and placement of dental implants.
If you have signs or symptoms that may be indicative of gum disease, please know this disease will only worsen without treatment. Call 828-274-9440 to schedule an appointment or ask to begin with a consultation.
If dental fear is a concern, we can discuss oral or IV sedation options. These are administered safely with skilled staff members who use advanced safety equipment throughout your care.
Additionally, if you’ve delayed care due to cost, we office several payment plans that many patients find helpful. These plans can break costs into monthly payments, often with no down payment required.
Sources:
https://www.nidcr.nih.gov/health-info/oral-hygiene
https://www.nidcr.nih.gov/research/oralhealthinamerica/section-2b-summary
https://www.nidcr.nih.gov/research/oralhealthinamerica/section-3b-summary
https://www.nidcr.nih.gov/research/oralhealthinamerica/section-3a-summary
https://www.womenshealth.gov/a-z-topics/oral-health
https://www.cdc.gov/tobacco/data_statistics/fact_sheets/adult_data/cig_smoking/index.htm
What Gum Disease Bacteria Does To You That May Surprise You.
Posted on Dec 15, 2023 by William J. Claiborne, DDS MS
As we round the corner of another year, making oral hygiene a priority seems a distant thought in the midst of holiday preparations and activities of the season. But, it should be at all times in our lives, for many reasons.
Over the years, research has continuously shown that the bacteria of periodontal disease can have a number of harmful effects – in the mouth AND elsewhere.
This is because these inflammatory bacteria can enter the bloodstream and travel throughout the body. Studies show that these bacteria can activate or worsen a number of serious health problems.
People easily understand that a mouthful of bacteria can cause bad breath and gums that may be tender and redden in color. This makes sense, since an area with a skin cut can redden and swell if it doesn’t heal properly. Yet, because gum tissues are concealed behind cheeks and lips, it is easier to ignore problems that may be clear that something is wrong if more exposed.
To be clear, bacteria in our bodies is not always a bad thing. For example, certain bacteria in the gut actually enhance the process of digestion and help to keep the digestive system operating efficiently.
However, some bacteria are bad. These ignite when too much bacteria invade the body, causing the immune system to become overburdened. Bacterial overload can leave the body’s natural defense response, white blood cells, unable to conquer the infection. So, when a cut becomes infected, your doctor may prescribe an antibiotic to give the immune system added reinforcements.
And, when bacteria overload occurs in the mouth, an inflammatory reaction begins. This is the beginning of gum disease.
Signs of gum disease include bleeding or sore gums, persistent bad breath, receded gums, and/or gums that are red rather than a healthy pink. These are warning signs since gum disease will only worsen without treatment.
As gum disease progresses, gums begin to pull away from the base of teeth, gums become very tender and bleed easily when brushing, pus pockets form on gums and teeth may shift or loosen.
Unfortunately, gum disease is ignored too often by adults in the U.S. The CDC estimates that over 47% of Americans have some level of gum disease, which is also the leading cause of tooth loss.
A periodontist is a specialist in the treatment of all stages of gum disease and in the placement of dental implants. He or she is the expert who can help to restore a bacteria-burdened “oral cavity” to a healthy state.
In addition to a healthy smile, the health of your gums can impact your overall health. By keeping the bacteria of advanced gum disease, known as periodontitis, you lower your risks of a long list of serious health problems that have been shown connected to gum disease bacteria. These include:
• Heart Disease & Stroke – According to research, having advanced gum disease makes you twice as likely to develop heart disease. This is due to clot-causing proteins that occur from oral bacteria that can clog arteries, including the carotid artery that supplies the brain with blood.
• Dementia & Alzheimer’s disease – Studies have shown that tooth loss from oral bacteria is a risk factor for memory loss and early stage Alzheimer’s disease. Apparently, oral infection cause inflammation triggers that can lead to the destruction of brain cells.
• Cancer – Researchers found that males with gum disease are 54% more likely to develop pancreatic cancer, nearly 50% more likely to develop kidney cancer and 30% more likely to have blood cancers.
• Diabetes – Because people with diabetes are more susceptible to infections, with 95% of whom also have periodontal disease.
• Erectile Dysfunction – Men with periodontal disease are 7 times more likely to have erectile dysfunction (ED).
• Premature Birth – Nearly 13% of U.S. babies are born premature, which can lead to breathing issues and infections. Infection in the mother’s body, which includes infection from periodontal disease, can create inflammatory reactions that are related to premature and low birth weight babies.
• Infertility – Research has found that gum disease can complicate attempts for a female to become pregnant.
• Respiratory Problems – When bloodborne bacteria from gum disease reaches the lungs, people with respiratory problems are at higher risk of pneumonia and acute bronchitis (COPD).
It has been said that the mouth is the gateway to the body. Whether it’s the holidays or vacation time or just a busy schedule, your oral health should be a commitment. It takes just minutes a day to brush your teeth thoroughly (at least 2 minutes each time), twice daily, floss daily and swish after meals.
Drink plenty of water, especially after consuming caffeinated beverages or alcohol (including wine). If you smoke, begin with a periodontal exam and ask our hygienist for at-home care instructions.
Call 828-274-9440 if you have questions about your gums or if you are experiencing any of the above mentioned symptoms of gum disease. Also, visit our website to learn more about our sedation options (including “twilight sleep”) and advanced technology, which often reduces treatment time while enhancing comfort.
A “Lecture-Free” Look At Cigarettes & Your Smile
Posted on Oct 11, 2023 by William J. Claiborne, DDS MS
In this article, I’m going to address cigarette smoking as it affects oral health. This is not intended to lecture or chastise an adult for making a choice to smoke or those caught up in the addictive grip of nicotine. My goal is to relay factual information regarding oral health for smokers so they can better protect their smiles.
Because I’m a native North Carolinian, I’ll begin by sharing some information on our State, as provided by 2018 stats from the CDC (Centers for Disease Control & Prevention).
In 2018, the percentage of adults in North Carolina who smoked was reported as 17.4% (of every 100 adults). The CDC shared findings of all states, with smoking ranged from nearly 9 of every 100 adults in Utah (9.0%) to 25 of every 100 adults in West Virginia (25.2%).
They also shared that cigarette smoking was lowest among those with a graduate degree (3.2%) and highest for those who had only achieved a GED certificate (30.7%). Those with a high school diploma showed a lower percentage of nearly half of the GED level adults at 17.1%.
As an Asheville periodontal dental specialist, smoking is a particular concern since many people are unaware of the oral health risks. While many smokers are familiar with the risks smoking poses related to cancer and other diseases, smoking is also terribly harmful to your smile.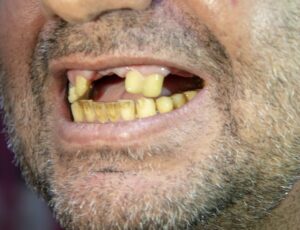
For instance, smokers have a greater risk of periodontal (gum) disease. The drying effect that smoking has on the soft tissues in the mouth offers an ideal breeding ground for oral bacteria. This enables easier entry of oral bacteria into the structures that support tooth roots.
According to the Centers for Disease Control & Prevention (CDC), a smoker has twice the risk for gum disease compared to that of a nonsmoker.
As oral bacteria thrive and reproduce in the mouth, gum tissues become tender and inflamed. These are signs of gingivitis, the beginning stage of gum disease.
Gum disease at this stage can cause persistent bad breath, swollen gums and gums that bleed easily when brushing. As it progresses, gum tissues turn red or purple from inflammation. Pus pockets may form at the base of some teeth. This advanced stage is known as periodontitis.
Eventually, the infectious bacteria penetrate below the gum line and attack supporting bone and the tissues surrounding tooth roots. This can cause teeth to loosen and eventually require removal. Gum disease is the nation’s leading cause of adult tooth loss.
Losing teeth is detrimental to your overall health and not a normal part of the aging process. Studies have shown that people who wear dentures die an average of ten years earlier than those who keep their natural teeth.
Denture wearers also have higher incidences of pneumonia, and worse. A 2015 report by NBC News shared findings surrounding dentures and MRSA biofilm. The report included a dental specialist’s warning that, “Concern about biofilms on dentures is growing as researchers continue to identify links between oral bacteria and heart disease, chronic obstructive pulmonary disease or COPD, and respiratory diseases, including aspiration pneumonia.”
Many smokers are aware that they have stained teeth and more-frequent bad breath than non-smokers. They also have slower healing periods after procedures such as extractions, gum treatment and oral surgery.
Although a hygienist may go slowly and gently, dental cleanings are typically less comfortable for smokers. This is because smoking causes a greater buildup of plaque. With gum tissues already tender from the bacterial irritation of plaque, removing buildup from between and around the base of teeth adds to the discomfort of inflamed tissues.
According to the American Dental Association (ADA), smoking increases the risks of oral cancer, lesions inside the mouth, enamel erosion and tooth loss in addition to periodontal (gum) disease.
If you vape, remember that nicotine in any form is a hazardous force in the mouth. And the vapor itself is not safe for oral health.
Vaping (using e-cigarettes) delivers nicotine through an inhaled mist. Although the vapor is generally not labeled as “dangerous,” one study of some e-cigarette products found the vapor contains known carcinogens and toxic chemicals, including, propylene or polyethylene glycol, glycerin, and additives. And, its nicotine is no less harmful to the user as that delivered via cigarette smoke.
Unfortunately, many cigarette users switch to vaping based on the perception that “e-cigs” are a safer alternative. For those hoping to wean themselves off cigarettes through this switch, very few achieve that goal as a result.
A 2018 report by the National Academy of Sciences, Engineering, and Medicine concluded there was “evidence that e-cigarette use increases the frequency and intensity of cigarette smoking in the future.”
Although the focus in this article is meant to be on oral health, allow me to reiterate some of the benefits of “kicking the habit” …
• Smokers have a decreased life expectancy of an average of 10–15 years compared to non-smokers.
• Smoking is linked to nearly a third of all cancer diseases and deaths.
• Pregnant women who smoke have a higher risk for first-trimester spontaneous abortion, preterm births, low birth weight babies and sudden infant death syndrome (SIDS).
• Women who smoke are at risk for early menopause while men who smoke are more at risk for impotency.
• People who breathe in your “second hand” smoke (what you exhale) are subjected to over 50 known carcinogens and other harmful chemicals.
For those who are able to give up smoking, the effort is well worth it. The positive effects can be felt almost immediately. In about 48 hours, damaged nerve endings begin to restore. The sense of smell and taste begin to return to normal.
“Quitters” also notice their breathing is easier in about 3 days and they have fuller air intake. Oral health improves within 2 weeks as blood circulation in the gums and teeth returns to nearly that of non-smokers. Heart attack risk also declines with blood flow greatly improving. Activities are easier and the constant smokers cough is gone.
 In our Asheville periodontal office, our goal – for every patient – is to help each achieve optimal oral health and a smile he or she is proud to share. For those who smoke, we make individualized recommendations so the potential for achieving this is favorable.
In our Asheville periodontal office, our goal – for every patient – is to help each achieve optimal oral health and a smile he or she is proud to share. For those who smoke, we make individualized recommendations so the potential for achieving this is favorable.
If tooth loss has already occurred, we are specialists in the treatment of all stages of gum disease and in the diagnosis and placement of dental implants. We will be happy to discuss the dental implant system that may be best for your needs.
Or, if dental fear or anxiety have kept you from receiving regular dental care, ask us about oral or IV sedation (“twilight sleep”). These sedatives are delivered by an MD of anesthesia for your optimal safety and comfort. And, in all procedures, we make patient comfort a high priority.
Call 828-274-9440 to schedule an examination.
Sources:
https://www.cdc.gov/tobacco/campaign/tips/diseases/periodontal-gum-disease.html
https://www.sciencedaily.com/releases/2016/11/161116101821.htm
https://www.nbcnews.com/healthmain/dirty-dentures-dangerous-mrsa-may-be-lurking-dentists-say-662637
https://www.cdc.gov/tobacco/basic_information/e-cigarettes/index.htm
Recent Posts
Categories
Archives
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- August 2014
- July 2014
- June 2014
- May 2014
- April 2014
- March 2014
- February 2014
- January 2014
- December 2013
- November 2013
- October 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- April 2013
- March 2013
- February 2013
- January 2013
- December 2012
- November 2012
- October 2012
- September 2012
- August 2012
- July 2012
- June 2012


