Header logo
header top contact widget
Oral Cancer
Gift Ideas For “Priceless” Smiles!
Posted on Sep 25, 2024 by William J. Claiborne, DDS MS
 It’s not even October and already I’m seeing holiday sales ads and decor. This comes across as pretty confusing when Christmas items are mixed into Halloween candy and skeleton costumes.
It’s not even October and already I’m seeing holiday sales ads and decor. This comes across as pretty confusing when Christmas items are mixed into Halloween candy and skeleton costumes.
However, Americans are wise to get a jump on the holidays since the rush of the Christmas season can become overwhelming. A long holiday shopping list can often be more manageable by jumping on early sales, saving time and money. Like every list, though, there is always that hard-to-buy-for person. At Biltmore Periodontics in Asheville, we have a suggestion…
An electric toothbrush can do a lot more than help an individual enjoy fresh breath and a bright smile. Studies have shown that brushing teeth with an electric version promotes better gum health and slower progression of periodontal (gum) disease. Compared to manual toothbrushing, an electric toothbrush can help to reduce the risk of tooth loss.
As part of a thorough at-home oral hygiene regimen, the thoroughness of an electric toothbrush was monitored in one study (published by the Journal of Clinical Periodontology). In this, the oral health of over 2800 adults was tracked for over 11 years. The use of electric toothbrushes was monitored to watch for periodontal disease, cavities, and the number of natural teeth.
From 2002 – 2006, participants were examined with follow ups conducted after 6 and 11 years. Eighteen percent of the participants were electric tooth brush users. At the time of their 11 year follow up, 37% had switched to using electric toothbrushes.
The study showed electric brushing promoted better gum health and slower progression of gum disease. Electric tooth brushing is also related to a reduction in tooth loss by 20% (compared to those who brush with manual toothbrushes).
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6619286/
One reason for the superior level of cleaning by an electric toothbrush is attributed to features of some models. Many of the newer models include a timer to indicate how long to spend brushing in each quadrant (your teeth divided into 4 sections). The timers are also helpful in the recommendation of brushing for at least two minutes twice daily. (This applies to both manual brushing or with an electric.)
Gum disease is the nation’s leading cause of adult tooth loss and one of the most prominent diseases in the U.S., with over 47% of adults having some level. Signs of gum disease include tender gums that bleed easily when brushing, gums that darken in color to red (versus a healthy pink), persistent bad breath, and gums that pull away from teeth (receded gums) and expose darker root areas of teeth.
As devastating as tooth loss is, the infectious oral bacteria can enter the bloodstream through diseased gum tissues. They are able to create inflammatory reactions that have been associated with a long list of health problems.
Decades of research have shown the bacteria of gum disease are able to trigger the onset of or worsen the development of severe (and even deadly) health conditions. These include: heart disease, stroke, high blood pressure, some cancers, diabetes, arthritis, impotency, preterm babies, dementia, Alzheimer’s disease, and more.
Thus, the gift of an electric toothbrush to a smile you love can improve that person’s oral health and help them in their overall health as well! As a periodontist, I have a firsthand view at how these can help greatly when it comes to time spent at the bathroom sink!
Another gift suggestion is an electric water flosser.
 Daily flossing is highly recommended for gum health, lower cavity risk and the prevention of tooth loss. Flossing removes trapped bits of food remaining in the mouth, which feeds oral bacteria and allows them to quickly multiply. Because brushing cannot dislodge all food particles caught between teeth, flossing should be a must-do in one’s daily oral hygiene routine at home.
Daily flossing is highly recommended for gum health, lower cavity risk and the prevention of tooth loss. Flossing removes trapped bits of food remaining in the mouth, which feeds oral bacteria and allows them to quickly multiply. Because brushing cannot dislodge all food particles caught between teeth, flossing should be a must-do in one’s daily oral hygiene routine at home.
Proper flossing is easy for those who are in the habit and takes only a minute each day. While an estimated 40% of American adults “claim” to be daily flossers, that’s disputable. Some polls show that about 37% admit they actually floss less than daily with just over 32% saying they never floss.
https://www.usnews.com/news/articles/2016-05-02/how-many-americans-floss-their-teeth
For those who have problems with manual dexterity or find the maneuver awkward, water flossers are an effective alternative. They are easy to use and have been found to be just as effective as manual flossing.
A water flosser works by pulsating a stream of water between teeth that is forceful enough to dislodge trapped food bits but without harming teeth or gums. The pressure can also be adjusted for one’s comfort. They can be affordably purchased online or in many stores.
While adults are gaining a better understanding of how the health in their mouths impacts their overall help, we believe that – like anything – having the right tools can create a stronger commitment and positively support an individual in doing the job effectively. Because every smile gives back so much, protecting it – or helping someone protect theirs – is a gift that has lifelong benefits.
If signs or symptoms of gum disease are suspected, call 828-274-9440. If dental fear or anxiety is a concern, we can discuss comfort options, including oral and IV sedation (“twilight sleep”).
If regular dental care has been difficult for you in the past, consider starting with a consultation. You’ll find the entire team at our state-of-the-art Asheville periodontal dental office treat patients with respect, compassion and a gentle touch.
New patients are always welcome and referrals are not always required.
Alzheimer’s Disease, Dementia and Periodontal Disease
Posted on Aug 15, 2024 by William J. Claiborne, DDS MS
In information posted on the web site of the Alzheimer’s Association (www.alz.org),
“A recent analysis led by National Institute on Aging (NIA) scientists suggests that the bacteria associated with periodontal disease that causes the chronic inflammation are also associated with the development of Alzheimer’s disease and related dementias, especially vascular dementia.”
 Is there a more dreaded disease today than Alzheimer’s? Not only is the individual effected, entire families are devastated when dealing with a loved one’s diagnosis.
Is there a more dreaded disease today than Alzheimer’s? Not only is the individual effected, entire families are devastated when dealing with a loved one’s diagnosis.
In the U.S., it is the 6th leading cause of death.
https://www.alzheimers.net/resources/alzheimers-statistics/
By the year 2025, the number of people 65 and older with Alzheimer’s disease is expected to reach 7.1 million people, a 27% increase from the 5.6 million over the age of 65 in 2019.
In 2020, it was estimated that 11.6% of North Carolina adults aged 65 and over had some level of the disease. Currently, 10% of American adults 65 and over have Alzheimer’s disease. For people ages 85 and older, this increases to 32%.
By 2060, nearly 1 in 4 Americans will be 65 years and older with seniors over age 85 having tripled.
https://www.alz.org/media/Documents/alzheimers-facts-and-figures.pdf
As a periodontist in Asheville NC, I’ve been following the findings related to Alzheimer’s disease and periodontal disease. Yes, the connection between the two seems far-fetched, but research is showing there is a correlation.
First, allow me to explain periodontal (gum) disease. Gum disease is an inflammatory disease that attacks gum tissues, teeth, and the structures that support them. It is the nation’s leading cause of adult tooth loss. In addition to the problematic oral symptoms associated with gum disease, research has shown that the infectious bacteria are able to activate the development (or worsen the progress) of other diseases.
Because the bacteria of gum disease are able to enter the bloodstream through weakened oral tissues, studies have connected them to serious reactions elsewhere in the body. Some of these lead to the formation of cancer (oral, throat, pancreatic, lung) and some activate conditions such as diabetes and arthritis.
While the statistics of aging adults increase, nearly half of the adult population has some level of gum disease, over 47%. As a periodontal specialist in Western NC, I believe the high prevalence of gum disease among U.S. adults may be, in part, due to the assumption, “if it doesn’t hurt, nothing is wrong”. People also tend to brush off some symptoms as “normal,” such as seeing blood in the sink when brushing teeth.
Although symptoms of gum disease may include tender gums that bleed when brushing, gum disease can begin without any obvious signs. One study included over 8,200 adult at an average age of 63 at the study’s onset. The findings showed an increased propensity for developing dementia for participants who had severe gum disease and missing teeth.
Having no natural teeth was associated with a 26% increased risk. At the end of the study:
• 14% of individuals with healthy gums and all their teeth at the start of the study developed dementia by the end of the study
• 18% of participants with mild gum disease developed dementia
• 22% with severe gum disease (periodontitis) developed dementia
• 23% of those with no remaining teeth developed dementia
Eighteen years later, a follow-up study found those who had severe gingivitis in addition to tooth loss had a 22% higher risk for developing Alzheimer’s disease or dementia.
What researchers found is the bacteria present in periodontal disease are able to travel through the mucous membranes of the mouth to the brain. This is believed to cause potential brain damage.
Now, more than ever, maintaining a healthy smile is important for every adult. If you suspect you have gum disease (gums that bleed when brushing, tender or swollen gums, gums that have reddened or receded from teeth), be seen by a periodontist. This disease will only worsen without treatment.
Be committed to having excellent oral health as and make it a priority as an important part of your overall health. For a consultation to discuss how we can help you achieve optimal oral health, call 828-274-9440.
In addition to the treatment of all stages of gum disease and the reshaping of gum tissues, a periodontist is a specialist in the placement of dental implants. If you have lost teeth, dental implants are the ideal tooth replacement option.
Also, please know that our Asheville periodontal dental office offers many comfort options, including Oral and I.V. sedation. Oral sedation is a pill that helps patients relax. I.V. sedation (also known as ‘twilight sleep’) places the patient in a deeper sleep state and erases memory of the procedure. It is administered by a doctor of anesthesiology for optimal comfort and safety.
Connections of Oral Wellness and Overall Health
Posted on Aug 08, 2024 by William J. Claiborne, DDS MS
Over the past few decades, an increased number of studies have pursued the many connections of periodontal (gum) disease and our overall health. With the findings, research has become more focused with links found between infectious oral bacteria and a growing list of serious health problems.
Periodontitis is the most severe form of periodontal disease. It is a severe form of gum infection that damages soft tissues and destroys the bone that supports teeth. This occurs when toxins produced by the bacteria in plaque irritate the gums.
These toxins activate a chronic inflammatory response in which the body, which turns on itself. This systemic inflammation leads to break down and destruction of tissues and bone that support the teeth.
The potent bacteria of gum disease are able to enter the bloodstream through tears in weakened tissues. It is now known that it can trigger inflammatory reactions that are related to the development of the conditions mentioned above. While it can activate the development of serious health problems far beyond the mouth, it can also worsen others already underway.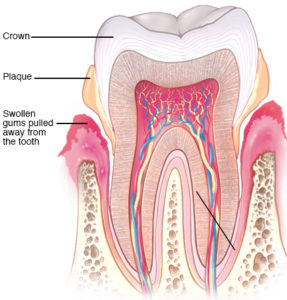
The initial stage of periodontal disease is gingivitis. This may have mild symptoms or even some deemed “normal.” These include areas where the gums are tender or seeing blood in the sink when brushing teeth. However, gingivitis, if not halted, can soon progress to periodontal disease.
Gum disease symptoms include:
• Gums that loosen from teeth (or “recede”)
• Red or swollen gums
• Gums that bleed when flossing or brushing
• Persistent bad breath
• Teeth that may loosen or drift
Without treatment, gum disease worsens. Many people are unaware of the severity of damage capable by these infectious bacteria. Below are some of the correlations that may surprise you.
Using findings from previous research, studies have closely scrutinized two types of oral bacteria pathogens. Researchers found that one pathogen was far more prevalent in the saliva of participants who developed pancreatic cancer with a 59% increased risk of developing the deadly cancer. Just as alarming was that the second pathogen was shown to increase this risk by 50%.
The connections between periodontal disease and other diseases in the body also include a link between oral health and psoriasis. Psoriasis is a chronic disease that affects the skin. Its cause isn’t fully understood but seems to relate to the immune system turning on itself.
This condition causes the life cycle of skin cells to accelerate beyond normal. Cells build up rapidly on the skin’s surface, forming scales and red patches that are often itchy and sometimes painful.
In one study, researchers found that while “people with psoriatic arthritis had about the same rate of gum disease as those without joint inflammation, people with psoriatic arthritis were more likely to have severe gum problems.”
https://www.psoriasis.org/advance/prevention-tips-for-uveitis-stroke-and-gum-disease
Other studies have shown that people with periodontitis (advanced gum disease) are nearly 1.5 times more likely to develop psoriasis than people with healthy gums. Could one trigger the other, and vice versa?
Another study showed that 36% of people with psoriasis had one or more sites of bone loss measuring at least 3 millimeters (over a tenth of an inch). This was compared to 13% of people without psoriasis.
For people who have rheumatoid arthritis (RA), many are learning that research is noting close connections with arthritis and gum disease, too.
RA is a debilitating, painful disease that destroys joints. RA often emerges gradually, initially causing morning stiffness and weak, sore muscles. As inflammation from RA worsens, joints become swollen. Joints become achy and stiff most often in the fingers, wrists, elbows, hips, knees, ankles, toes, and neck. Unfortunately, there is no cure for RA.
Apparently, gum disease and RA share a genetic similarity. The clinical makeup shows similar structures, primarily in pathogens that spark disease or illness. Research has found that the pathological process that occurs in both gum disease and RA are nearly identical.
Both conditions cause chronic inflammation in tissues that connect to bone with both diseases having a similar inflammatory trigger. Even more similar is the particular species of bacteria found in periodontally-diseased tissues when compared with tissues around arthritic joints. In one study, a particular pathogen associated with periodontal disease was found to activate the same destructive process of rheumatoid arthritis.
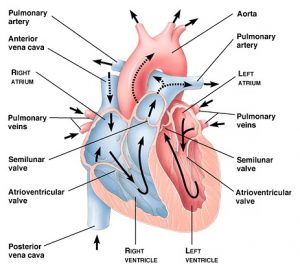 Another example of damage possible by the infectious bacteria of periodontal disease is coronary artery disease. The heart disease connection, as explained by Harvard Medical School’s newsletter, states:
Another example of damage possible by the infectious bacteria of periodontal disease is coronary artery disease. The heart disease connection, as explained by Harvard Medical School’s newsletter, states:
“In people with periodontitis (erosion of tissue and bone that support the teeth), chewing and toothbrushing release bacteria into the bloodstream. Several species of bacteria that cause periodontitis have been found in the atherosclerotic plaque in arteries in the heart and elsewhere. This plaque can lead to heart attack.
“Oral bacteria could also harm blood vessels or cause blood clots by releasing toxins that resemble proteins found in artery walls or the bloodstream. The immune system’s response to these toxins could harm vessel walls or make blood clot more easily. It is also possible that inflammation in the mouth revs up inflammation throughout the body, including in the arteries, where it can lead to heart attack and stroke.”
http://www.health.harvard.edu/press_releases/heart-disease-oral-health
And the list goes on, even including connections between periodontal disease and erectile dysfunction (ED). For men in the 40 – 70 age group, ED affects over 40% with nearly 70% of men at age 70 affected.
One study of 162 males ages 30 to 40 by Turkish researchers, 82 of the participants had normal erection function while 80 who complained of ED, nearly half. Some men in both groups had chronic periodontitis, but the condition was more than twice as prevalent in the ED group.
In another study, 80 male participants who had severe gum disease were more than twice as likely to suffer from erectile dysfunction. This was true even after adjustments were made for other issues that could distort the findings.
Gum disease affects nearly 47% of American adults. It will worsen without treatment and, to no surprise, is the nation’s leading cause of adult tooth loss. As an Asheville periodontal specialist, I have an up-close view of the damaging effects of gum disease.
If you are experiencing signs of gum disease, start with a thorough periodontal examination. Call 828-274-9440 or ask our friendly staff about beginning with a consultation.
If dental fears have caused you to delay or avoid having regular dental care, many treatments can include oral or I.V. sedation (sleep dentistry, or “twilight sleep”).
And, if financial constraints are an obstacle in receiving treatment, we offer several payment plans. Most are interest-free with no down payment required (for qualified individuals). Feel free to ask about these during your consultation.
Know How Summer Comes With Oral Health Risks
Posted on May 20, 2024 by William J. Claiborne, DDS MS
As an Asheville periodontist, there are two times a year I feel come with higher risks for keeping one’s oral health well-maintained.
One is during the Thanksgiving-Christmas season. During these times, people tend to consume food and beverages that are higher in carbs and simple sugars. And, they eat more frequently. I understand – it’s pretty hard not to sneak a piece of grandma’s fudge with a mid-morning cup of coffee!
Although the hardships to teeth and gums brought on by these indulgences may be diluted by swishing or an extra brushing during the day, summertime has its own set of challenges that are rather similar.
First, understand that any time you eat or drink something (other than plain water), an acid attack begins in the mouth. This acid flows in with saliva, bringing in an acid to break down food as its chewing; the body’s first stage of digestion. These acids are rather potent in that they can even soften enamel for 20-30 mins. Thus, when other acidic elements are introduced in the mouth, the higher levels of acid can leave precious tooth enamel at risk.
Below are things to keep in mind as we go into the official “it’s okay to wear white” season!
Oral acidity – Summer foods and beverages seem to come with a wealth of consumables that are high in acidity – garden fresh tomatoes, lemonade, water or tea with a squeeze of lemon, etc. Just know that they need to be diluted by swishing with water or drinking gulps of water while consuming.
Colas – I can’t say enough bad things about colas when it comes to oral health. While sodas, coffee, tea and wine are all highly acidic, the acidity levels in colas have been compared to nearly that of the levels in battery acid. Colas are highly acidic because they are infused with phosphoric acid, intended to add flavor. Phosphoric acid is so erosive it can remove rust from aircraft carriers and ships.
When these erosive acids are mixed with the acids that occur naturally in the mouth, there is a significantly higher potential to erode tooth enamel. Dental erosion can cause temperature sensitivity, pain, transparent teeth, cracking and darkening of teeth.
Also concerning is the way colas are consumed. Every time you sip a soda, an acid attack in the mouth is triggered for 20-30 minutes until eating or drinking ceases. Because colas are typically consumed slowly over long periods of time, the acid attack lasts that long plus another 30 minutes before subsiding. For colas containing sugar, this mixes with the acid in the drink and your digestive acids for an even greater level of destruction.
Accidents & injuries to the mouth – Outdoor sports and activities such as skiing, biking and baseball should all be done with a custom-made mouthguard in place. This is important for children and adults. Having a permanent tooth knocked out can be devastating.
If the worst should happen, a periodontist is your specialist in placing dental implants. And, by acting soon after the tooth is lost, you can preserve the natural contours of the gum tissues that arch the tooth. These arches of gums help to create a natural appearance when the replacement tooth is placed along with the “points” that dip slightly between each tooth.
A periodontist has advanced skills in the diagnosis and placement of the implant type best for individual needs. In our Asheville periodontal dental office, we use advanced imaging and implant guidance technology that helps to minimize treatment and optimize comfort with reduced healing time.
Oral Dryness – “Dry mouth” promotes oral bacteria by enabling rapid reproduction. When oral bacteria are able to linger in the mouth, they have an ideal warm, dark, moist environment. Without saliva serving as a continual rinsing agent to keep bacteria levels in the mouth under control, oral bacteria accumulate at a rapid pace.
Water intake helps to support saliva in the mouth to rinse bacteria and food particles from the mouth. Sufficient saliva flow helps in neutralizing the acids produced by oral bacteria and aids in preventing tooth decay and the development of periodontal (gum) disease.
By understanding where the risks lie, you can take proactive measures between visits to prevent things like cavities and gum disease.
An overload of oral bacteria initially reveals itself as plaque, at first. This is a sticky film that coats the teeth and gums, which is easily noticeable upon waking up. If not thoroughly removed each day, it can hardened at the base of teeth. This is known as tartar.
Tartar is a cement-hard colony of bacteria, which feed on tender gum tissues. This can cause tender gums that bleed easily when brushing and more frequent bad breath.
This early stage of gum disease is known as gingivitis. If not resolved quickly, it can easily progress. Periodontal disease is an inflammation of the gum tissues that causes bleeding, swelling, persistent bad breath and gum recession. As it worsens, gum disease can enter the advanced stage of periodontitis. In this, infectious oral bacteria attack the area below the gum line, including bone and tissues that support natural teeth.
The bacteria can also enter the bloodstream through tears in diseased gums. The inflammatory nature of this bacteria can trigger a number of serious health problems, including heart disease, stroke, some cancers, diabetes, arthritis, pre-term babies and more. Periodontal disease is also the nation’s leading cause of adult tooth loss.
Summer is a wonderful time for vacations and being more active outdoors. However, don’t let your daily oral care regimen result in costly repairs down the road. Avoid taking “time off” from your twice-a-day oral hygiene routine so bacterial growth doesn’t require dental treatment as a result.
When vacationing, some tips for your oral upkeep include:
• When packing, place your tooth brush, floss and toothpaste in one container separate from other items. Once you arrive at your destination, place this by the sink so they are handy each morning and evening.
• Take along sugarless gum to help you maintain sufficient saliva flow in the mouth. This aids in removing bacteria before it builds into the stick film that forms plaque.
• Brush at least 2 minutes per brushing followed by brushing your tongue to dislodge embedded bacteria.
• If you can’t brush right after a meal, swish with water or chew sugarless gum.
• Drink lots of water throughout the day to keep oral tissues moist.
Call 828-274-9440 if you have questions about your gums or if you are experiencing symptoms of gum disease. This disease will only worsen without treatment. You may also wish to begin with a consultation.
You are invited to visit our website to learn more about dental implants, sedation options (including “twilight sleep”) and advanced technology.
Recent Posts
Categories
Archives
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- August 2014
- July 2014
- June 2014
- May 2014
- April 2014
- March 2014
- February 2014
- January 2014
- December 2013
- November 2013
- October 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- April 2013
- March 2013
- February 2013
- January 2013
- December 2012
- November 2012
- October 2012
- September 2012
- August 2012
- July 2012
- June 2012


