Header logo
header top contact widget
Blog Archives
Recent Posts
Categories
Archives
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- August 2014
- July 2014
- June 2014
- May 2014
- April 2014
- March 2014
- February 2014
- January 2014
- December 2013
- November 2013
- October 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- April 2013
- March 2013
- February 2013
- January 2013
- December 2012
- November 2012
- October 2012
- September 2012
- August 2012
- July 2012
- June 2012
Dental Fear Can Lead To Gum Disease, Tooth Loss
Posted on Nov 23, 2021 by William J. Claiborne, DDS MS
Fear is a natural reaction to things that may harm us; it’s a safety mechanism activated by the brain. Take snakes, for instance. Even harmless snakes tend to provoke an initial reaction that warns of impending danger.
Some fears are learned, however. Some people are afraid of dogs, usually stemming from a frightful encounter as children. The incident triggers something in the brain that reminds the individual, even into adulthood, that dogs are to be feared.
When it comes to the fear of dentistry, it often exists because of a traumatic incident in the patient’s past. Or, in some cases, it exists for unknown reasons. Too, certain smells, sounds or sights can trigger the “panicky” reaction some people have to dental visits.
As a periodontist in Asheville, I have a firsthand view of just what dental fear can do to oral health. Avoiding regular dental care is a sure recipe for cavities, periodontal (gum) disease, and eventual tooth loss.
Typically, adults who avoid dental visits feel they are doing an adequate job maintaining their oral wellness at home. In some minds, “I brush twice a day,” can be the justification to bypass recommended 6-month dental check-ups and cleanings.
Yet, even the best of at-home dental hygiene can be insufficient to the buildup of tartar.
Tartar is the hardened form of plaque, which is a sticky film of bacteria that accumulates in the mouth. In the form of tartar, this cement-hard mass of bacteria cannot be brushed or flossed away. It can only be removed by a dentist or hygienist using special tools.
While plaque can cause bad breath and a “furry” feeling mouth, tartar eats away at tender gum tissues and bores into tooth enamel. As it grows, it works its way below the gum line, creating inflammation in the gum tissues.
Early symptoms of gum disease, known as gingivitis, are tender or swollen gums. You may see blood in the sink when brushing teeth. Breath odor may be bad on a regular basis.
At this point, proper measures may be able to reverse the progression of these rapidly-reproducing bacteria. This requires thorough brushing (twice a day, at the very least), daily flossing, drinking lots of plain water, and using an oral rinse to control bacteria levels.
However, if tartar exists, it’s not going to go away. It will continue to amass and attack the gums and work its way into the tissues below. When the bacteria reach an uncontrollable level, they become infectious.
Think of gum disease bacteria as you would water in a pan on the stove. The heat will eventually cause bubbles to form on the bottom of the pan. This can be likened to gingivitis.
However, as the water heats more, bubbles start to move to the surface. This can symbolize the development of gum disease. The symptoms of gum disease include gums that turn red and bleed easily and persistent bad breath.
When advanced stage periodontal disease develops (periodontitis), imagine the water at full boil. Unfortunately, once aboil, the roil continues even after you remove the pan from the heat. This is known as systemic inflammation.
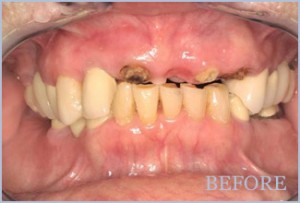
Gum disease is the nation’s leading cause of adult tooth loss. Yet, the bacteria that destroy gums and the structures that support natural teeth don’t remain confined to the mouth. Through tears in diseased gum tissues, these infectious bacteria can enter the bloodstream.
Research has correlated oral bacteria to a long list of serious health problems. Some can be activated by the bacteria of periodontitis, some are worsened. These include heart disease, stroke, Alzheimer’s disease, arthritis, diabetes, preterm babies, erectile dysfunction (ED), some cancers (including pancreatic), and more.
Obviously, these bacteria are potent and a threat to overall health. For those who avoid dental care due to anxiety or fear, knowing all this is not necessarily going to change their resistance. We understand that it’s still difficult to overcome the challenges even knowing there are risks.
There are options, however, for even high fear dental patients.
In our office, we offer I.V. sedation (“twilight sleep”) as well as oral sedation. Oral sedation is in pill form and creates a totally relaxed feeling. It enables patients to recover quickly and offers an amnesiac effect.
I.V. sedation is a deeper level of sedative. This places patients in a sleep state and erases most or all memory of the procedure after. With both sedations, however, we apply numbing medications to the area being treated to create optimal comfort for patients. We want patients to be in total comfort throughout their treatment, regardless of the addition of sedation.
We also have a reputation for treating our patients with respect and a gentle touch. We are just as committed to comfort for patients who do not want to be sedated as we are for those who are. Our goal is to help each person achieve a healthy, confident smile.
One of the most satisfying parts of my specialty is helping a once-fearful patient achieve a healthy, confident smile and see dental care as a welcomed part of their health care commitment.
If you are ready to get past your dental fears so you can have the smile you desire, begin by calling our Asheville periodontal office at: 828-274-9440 and speaking with our friendly staff. You can begin with a consultation, if desired.
Replace Teeth With Dental Implants Makes Good Sense
Posted on Nov 16, 2021 by William J. Claiborne, DDS MS
There’s a reason your general dentist is so determined to help you keep your natural teeth. When he or she recommends a crown (‘cap’) on a tooth to prevent potential removal (at the time or in the future), it is because a lost tooth is problematic in many ways.
First, the portions of teeth you see above the gum line stay in stable position because of the roots that hold it. Tooth roots (think “legs”) are supported by the upper or lower jaw bone. Larger teeth may have four roots. Some of the smaller teeth have only one.
These roots are beneficial to the health of the jaw bones. Tooth roots are connected to the jaw bone by veins and nerves that run from the tooth’s interior and out the bottom of each root leg. These vessels carry blood to the bone while providing a sort of stimulation that helps the bone to maintain its mass.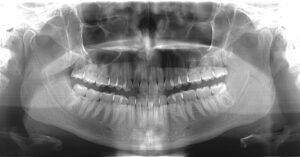
Think of the stimulation that tooth roots provide to how you might muscle atrophy. We all know that muscles, not used, will shrink in mass. When the jaw bones are lacking stimulation by the tooth roots they’re designed to hold, bone mass begins to decline.
Bone loss is the reason for a long line of problems. When bone loss occurs next to an area where natural teeth are held, those teeth are most likely to be the next to be lost.
When bone loss begins, it accelerates with each passing year. And eventually, a shrinking jaw bone reveals itself in changes in facial appearance. Initially, there may be deep wrinkling around the mouth. The corners of the mouth turn downward. Jowls form and the chin becomes more pointed.
As bone loss becomes more severe, the mouth seems to sink into the face. The nose and chin get closer, giving a “granny look”. The thin jaw bone is also more vulnerable to breaks.
Bone loss is what causes a change in how partials and dentures fit. As the bone height declines, the denture or partial becomes less secure from the declining bone shape to which it was designed to fit. More-frequent applications of pastes and adhesives are needed. Relines help but only temporarily.
Teeth also serve to support neighboring teeth. Each tooth keeps the ones on either side and above (or below) in proper position. This supports the “bite” alignment. A misaligned bite (how upper teeth fit and interact with lower teeth) can result in teeth that become chipped, worn or fractured.
Bite misalignment can also lead to TMJ disorder. The TMJ are your jaw joints, which hinge the lower jaw to the skull. When a misaligned bite causes stress or strain on these joints, the result can be headaches, sore jaw joints, ear ringing, vertigo, difficulty opening the mouth fully, and sore muscles in the face, neck and shoulders.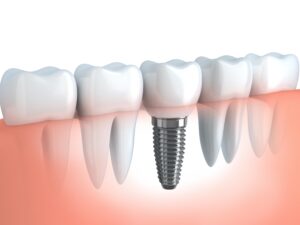
The reason we advise replacing teeth with dental implants are many:
1). A dental implant recreates the presence of a natural tooth. It provides stimulation to the bone, halting the process of bone loss.
2). Dental implants do not rely on neighboring teeth for support, as in a crown-&-bridge combination. The crowning of bordering natural teeth to support a bridge is not needed. Thus, the integrity of surrounding teeth is protected.
3). Because dental implants are supported by the jaw bone, sturdy and dependable biting and chewing strength is restored. Eating a healthy diet of all the foods you love is again possible.
4). Dental implants come in many sizes and shapes, each system designed to accommodate various needs and preferences. This means your implant can be chosen to suit your long-term goals.
5). Dental implants have an extremely high success rate, higher than any implant-in-bone option.
6). Dental implants are designed to last a lifetime. With proper selection and maintenance, they will never need replacing or repair. This makes them an excellent investment.
A periodontist is a dental specialist who is skilled offers an advanced understanding when it comes to oral tissues as well as dental implants. The advantages of a periodontist in dental implant selection and placement are many.
A periodontal specialist is trained to understand the intricate concepts involved in selecting the proper type of implant and skilled at placing implants at proper depths and angles. A periodontist is also able to optimize patient comfort during treatment and throughout the healing phase.
Using his or her advanced training in the diagnosis and placement of dental implants, a periodontist can help you enjoy a higher potential for dental implant treatment that lasts a lifetime.
In our Asheville periodontal dental office, we offer some of the most advanced technology available. This technology, combined with our advanced skill level, can help you enjoy a comfortable, efficient experience that allows you to have optimal success.
To learn more, call our office at: 828-274-9440 to request a consultation. Or, begin with an initial periodontal examination.
Mouth Sores – What Is Harmless & What To Watch Closely
Posted on Nov 04, 2021 by William J. Claiborne, DDS MS
As the holiday season approaches, our risk for illness goes up. Our chances for picking up colds or the flu increases, which is worrisome on its own. Add that to already-high concerns surrounding exposure to COVID, and we’re all taking added precautions to protect our health.
As in any year, colder months mean we’re more confined to the indoors and in closer proximity to others. With heightened potential for illness, the holidays simply create more stress to our lives. Stress is a contributor to our health as it compromises the immune system. This, in turn, lowers our resistance to fight off illness.
After the holiday mingling constraints endured in 2020, people are trying to take added precautions in 2021 so our “togetherness” is not overshadowed with worries about exposure to illness. To bolster our resistance, many people have had their Covid booster and flu vaccines, practice frequent hand washing, take vitamin supplements such as C, and are trying to stay active physically inside and out-of-doors.
Certainly, we applaud the health safety efforts taken by our Northwest NC population. As an Asheville periodontist, just a added tip for your overall health and well-being: Don’t forget to monitor the inside of your mouth while being committed to the other health measures you’re taking. You may be surprised at what your mouth reveals.
In busy times of year like the holiday season, we see a greater number of individuals who develop canker and cold sores. As stress goes up, your likelihood of getting a cold or canker sore increases as well.
The difference between Canker and Cold sores is:
Canker Sores
These are small ulcers that typically have a white or gray base and red border. Unlike cold sores, canker sores appear inside the mouth and are not contagious. The exact cause of canker sores is uncertain but fatigue, stress or allergies can increase the likelihood of a canker sore. Some experts suspect immune system problems, bacteria or viruses can also spurn eruption. A cut caused by biting the tongue or inside of the cheek as well as hot foods or beverages may contribute to canker sore development. Canker sores usually heal on their own in a week or two. Over-the-counter topical anesthetics, steroid preparations, and antimicrobial mouth rinses can provide temporary relief. As a holistic method, you may try swishing with plain, sugar-free yogurt for a minute or so. This helps to restore a healthy bacteria balance in the mouth while soothing discomfort.
Cold Sores
These are also referred to as fever blisters or Herpes simplex and are located around the lips, under the nose or on the chin. Caused by herpes virus type 1, cold sores are very contagious. These are clusters of fluid-filled blisters that often erupt since are they are most commonly found around the edge of the lips. Cold sores are Herpes lesions that may follow a fever, sunburn, skin abrasions or emotional upset. Because cold sore blisters are on the outside of the mouth, they can be embarrassing and uncomfortable. Although they usually heal in a week, over-the-counter topical anesthetics may speed the process while providing some relief. In our office, we can use a dental laser to hasten healing, often within a couple of days. If occurrences are frequent, ask about prescription drugs that can help reduce the duration of these viral infections.
Other issues your mouth’s interior can reveal include:
White Coating On Tongue
The tiny, bumpy protrusions on the tongue’s surface are papillae. Papillae are our source for taste and touch, allowing for feeling food’s form and texture. Saliva and food residue can become embedded in the grooves between the papillae, especially on the back portion of the tongue. This can create areas for rapid bacterial growth. As bacteria accumulate, a whitish film coats the tongue, which leads to bad breath. Let your white tongue be a warning sign of too much bacteria and take measures to manage it before cavities and gum disease develop. It’s important to keep the mouth moist since a dry mouth provides a breeding ground for bacteria reproduction. Drying sources, in addition to age, include smoking, alcohol consumption, caffeinated foods and beverages, and many prescription and OTC medications. Uproot bacteria in the tongue daily by brushing the tongue with your toothbrush after brushing teeth. Some toothbrushes have a tongue scraper on the back side of the bristles or you may want to purchase a tongue scraper. These are flexible strips you use to scrape over the tongue’s surface in a back to front motion.
Cheek Biting
Cheek biting can occur from a minor accident, such as during a fall. It can also occur from careless chewing or talking while eating. Cheek bites can occur more frequently due to a bite that is misaligned. A disparity in the bite can disrupt the harmonious congruency of upper and lower teeth while chewing and speaking. Cheek biting can be a symptom of bite misalignment. Other signs may indicate temporomandibular joint (or TMJ) disorders, which often result from a misaligned bite. Thus, cheek biting can be related. Too, TMJ disorders can cause night-time clenching or grinding of teeth. During these actions, you may be unknowingly biting the inside of your cheek while asleep. Cheek biting can cause inflammation at the location of the bite and can also result in canker sores. Chronic cheek biting can result in redness, painful sores, and tears in the mouth’s inner lining. Repeated bites can cause the oral tissues to become thick, scarred, and paler in the affected area. This surface can prompt the individual to continue biting in an attempt to create a smooth surface. If cheek biting has become habitual, there may be an emotional cause, such as stress, anxiety, depression, or even genetics. This should be discussed with your primary care physician.
Oral Cancer
It is important to pay close attention to any change to oral tissue that does not heal within 10-14 days. When oral tissue does not repair on its own in a week or so, it should be examined by your dentist or periodontist without delay. Some of these spots can be a symptom of oral cancer.
Oral cancer has one of the worst survival rates of all cancers. Because symptoms can mimic a bite on the inside of your cheek, more obvious symptoms often do not emerge until the cancer has reached advanced stages. Of those who acquire oral cancer, only 57% are estimated to still be alive 5 years later. Know the signs of oral cancer, which include:
• white or red patch of tissue
• unusual lesion in the mouth
• difficulty or discomfort when swallowing
• persistent sore throat or feeling something is stuck in the throat
• a lump or mass inside the mouth or neck
• wart-like mass
• numbness in the mouth or face
Lesions or discolorations that are early warning signs are not always visible, particularly in the back portion of the mouth. Because symptoms emerge slowly, the delay in early diagnosis and treatment can have deadly consequences. This reinforces the need to maintain regular oral hygiene exams and cleanings every six months. During these times, unusual changes in the mouth can be noted and, if concerning, further steps can be taken. Remember, never wait until your next dental check-up appointment to have anything unusual examined.
 Bleeding Gums
Bleeding Gums
Contrary to what some people believe, having gums bleed at any time is not normal. Seeing blood in the sink when you brush is not a sign you’re doing a good job. It’s a sign that the gum tissues are either being scrubbed too harshly or the gum tissues are infected by accumulated oral bacteria. If you notice bleeding – at all – take extra measures to maintain excellent oral hygiene at home. This includes twice daily brushing, daily flossing, using an oral rinse, keeping the mouth moist (ideally by drinking plain water), and limiting sugar. If bleeding continues for more than a couple of days, make a dental appointment. You may have developed Gingivitis, which is an early stage of gum disease. Halting this in its tracks early can save you greatly in treatment time and expenses.
The interior of your mouth can be a great indicator of your health in other areas. Just be sure to look inside and stay proactive on steps needed to keep the interior “in the pink”. Again, if an unusual spot or sore is still present after two weeks, call 828-274-9440 immediately for an appointment.


