Header logo
header top contact widget
grinding or clenching
What You May Be Doing To Increase Potential For Gum Disease
Posted on Apr 11, 2024 by William J. Claiborne, DDS MS
There’s a saying: “We don’t know what we don’t know.”
That applies to so much in life. With all good intentions, adults go about their days feeling they are doing what is right. However, we occasionally learn that what we thought was right is to our detriment.
For example, decades ago, people felt that rigorous scrubbing of teeth with a hard toothbrush and baking soda was a good way to clean your teeth. We now know that the hard bristles and abrasive substances can wear down tooth enamel and scrub away tender gum tissues.
And, there are ways that we actually – and unconsciously – add to the risks for developing periodontal disease.
Over the years, research has continuously shown that the bacteria of periodontal disease can have a number of harmful effects – in the mouth and further. Because these inflammatory bacteria can enter the bloodstream and travel throughout the body, research has shown that they can activate or worsen a number of serious health problems. These include:
– heart disease
– stroke
– Alzheimer’s disease and dementia
– arthritis
– diabetes
– preterm babies
– erectile dysfunction (ED)
– some cancers (including lung and pancreatic)
– obesity
Signs of gum disease include bleeding or sore gums, persistent bad breath, receded gums, and/or gums that are red rather than a healthy pink. These are warning signs since gum disease will only worsen without treatment.
As gum disease progresses, gums begin to pull away from the base of teeth, gums become very tender and bleed easily when brushing, pus pockets form on gums and teeth may shift or loosen.
Unfortunately, gum disease is ignored too often by adults in the U.S. The CDC estimates that over 47% of Americans have some level of gum disease, which is also the leading cause of tooth loss.
Bacterial overload can leave the body’s natural defense response, white blood cells, unable to conquer the infection. Thus, bacteria overload in the mouth triggers an inflammatory reaction begins, which is the beginning of gum disease.
Below are things that can increase the risk for gum disease, some of which you may not realize are contributors:
Aging: Studies have indicated that the incidence of periodontal disease increases as we get older. Over 70% of adults who are aged 65 and older have some form of gum disease.
Some Existing Health Problems: People who have diseases such as cancer or heart problems already have weaker immune systems. When the bacteria of gum disease enter the bloodstream through tears in oral tissues, harmful clotting factors and proteins can occur elsewhere in the body. Research has linked gum disease bacteria with heart disease, diabetes, stroke, preterm babies, and memory loss.
Dry Mouth: Smoking, certain medications, drinking alcohol and aging all contribute to a dry mouth. The saliva in your mouth plays an important part in removing food particles and bacteria. When insufficient saliva cannot cleanse the mouth adequately, bacteria buildup results.
Stress: It has been proven that people who endure long-term stress have a greater risk for developing diseases such as cancer, hypertension and even gum disease. Stress takes a toll on the body’s entire operation, weakening its ability to fight infection.
Medications: The side effects of some drugs can dry out oral tissues and even weaken the density of bones, opening the door for gum disease. Like your physician, your dentist should have an up-to-date list of all medications you take, including herbal supplements.
Grinding Teeth: When you grind and clench your teeth during sleep, the teeth wear down and connective oral tissues are weakened. When the tissues surrounding your teeth are vulnerable, your entire jaw bone area is exposed to certain infections, which can lead to gum disease.
Genetics: Because of genetics, you can be predisposed to develop gum disease. Research indicates that 30% of the population may be genetically susceptible to gum disease.
Gender: Periodontal disease occurs more in men than women (56% vs. 38%).
Smoking: Smoking dries out the tissues in the mouth, increasing one’s susceptibility to calculus. Research shows that smokers lose more teeth than nonsmokers and typically require longer healing times after treatment with results that are less predictable.
A periodontist is a specialist in the treatment of all stages of gum disease and in the placement of dental implants. He or she is the expert who can help to restore a bacteria-burdened “oral cavity” to a healthy state.

Dr. William Claiborne,
Biltmore Periodontics
In our Asheville periodontal dental office, we feature some of the most advanced technology in the industry. The patient benefits from these through diagnoses that are exact, more conservative treatment, and having reduced healing time. This also can mean there is less discomfort.
One of the features we provide is the LANAP Protocol Using Periolase MVP-7. LANAP (an acronym for Laser-Assisted New Attachment Procedure) is amazing technology that more efficiently and effectively treats periodontitis (advanced gum disease) with the PerioLase® MVP-7™ laser. As a minimally invasive (non-surgical) treatment for moderate to severe periodontal disease, LANAP has even been found to stimulate bone regrowth in damaged areas.
If you are experiencing symptoms of gum disease, call 828-274-9440. In our state-of-the-art Asheville periodontal dental office, our patients are treated with respect, compassion and a gentle touch. New patients are always welcome.
If dental fear has kept you from having regular dental care and you’re experiencing symptoms of gum disease, consider starting with a consultation. During this time, we can discuss comfort options, including oral and IV sedation (“twilight sleep”). Referrals are not required.
Avoid Dental Implant Failure
Posted on Apr 04, 2024 by William J. Claiborne, DDS MS
There are reasons to go to an expert for certain things. For example, I’d never try to do electrical work around my house on my own; I’d call an electrician.
When it comes to dental implants, there are also reasons to seek out an “expert.” In this article, I’ll explain why it’s best to have your dental implants selected and placed by a periodontist.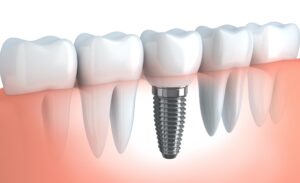
First, let’s look at the structure of an implant. Serving as a replacement for a missing tooth, the implanted portion is a titanium screw that is positioned into the jawbone. Over the course of 3-6 months, the jawbone grows around the implant, securing it in place. It can now support an artificial tooth or crown.
Dental implants have many benefits when it comes to restoring biting/chewing/speaking function and smiling appearance, including:
- enhancing the appearance of a smile
- improving biting and chewing function
- stabilizing surrounding teeth and jaw tissue
- halting the process of bone loss, known as resorption
- an increased quality of life for many people
Dental implants have an excellent success rate – 90-95%. However, there are instances where a dental implant can fail.
Dental implant complications can occur from infections, gum recession, and nerve and tissue damage. There is also a higher risk of implant failure for individuals who smoke or have diabetes, gum disease, have radiation therapy to the jaw area or take certain medications.
A periodontal specialist has advanced training and skills in the diagnosis and placement of all types of dental implants. This means that this dental specialist can determine which implant system will work best for your individual needs. For example, a person who has lost a great deal of bone mass may only be a candidate of certain implant types or may need a sinus lift prior to placement. A periodontist can make these determinations so your potential for implant success is higher.
One of the most common causes for implants failure is due to an infection at the implant site. Because a periodontist specializes in the care of gum tissues in the mouth, he or she can take measures to treat the infection at early stage to resolve the problem. However, in some cases, treating the infection may require implant removal in order to reach the infected bone tissue.
Using advanced skills, a periodontist can also assess your gum health prior to implant placement. He or she can pretreat any periodontal diseases so the implant has a healthy foundation. When the gum tissues around the implant are inflamed or have receded, the implant is at risk for entry of bacteria into the area where it is implanted.
After the implant is placed, it should fuse with the bone. A complication that prevents this may require the dental surgeon may remove it. Fortunately, after the implanted area is restored to a healthy state, the implant procedure can be redone.
Another benefit in using a periodontal specialist for implant placement is in their in-depth understanding of the nerves and tissues surrounding the jaw bones. There is a risk for failure when a dental implant is placed too close to a nerve. For example, there is a nerve that runs horizontally through the lower jaw. If the implant is placed in close proximity, it can cause numbness, tingling, or pain.
Nerve or tissue damages can result in:
-
- numbness on the side of the implant, including the lower lip and chin
- persistent pain or discomfort
- tingling, tickling, or burning sensations in the gums and skin
While precision placement (depth, position and angle) is a bonus of a periodontist’s skills for implant patients, our Asheville periodontal dental patients have the benefits of advanced technology. Our Computerized Dental Implant Placement system is designed for pre-surgical positioning of dental implants that uses a 3D model of the patient’s jaw.
Once the implant type is selected, a template is developed for optimal treatment success, even for complex cases. This minimizes disruption of gum tissues and targets implant placement at ideal depths and angles. Thus, treatment success rates are higher with faster (and more comfortable) healing time.
An example of this precision placement guidance in with upper dental implants. With declined bone mass of the upper jaw (typically from years of missing tooth roots), the sinus cavities can hover too close to the position(s) where implants are to be placed. In these cases, we can perform a sinus lift.
Should the dental implant protrude into the sinus cavity, the sinuses can become inflamed, causing:
- pain, tenderness, or swelling around the cheeks, eyes or forehead
- nasal blockage, often with green or yellow mucus
- a reduced sense of smell
- headaches
- toothache
- persistent bad breath
Of course, like a natural tooth, excessive force or impact can cause a dental implant to crack or become loose. For example, for people who grind or forcefully clench their teeth (“bruxing”) during sleep may need to wear a bite guard to prevent damage to the implant as well as their natural teeth.
In some instances, it can take up to 5 years for implant-related problems or infections to become apparent to the patient. Any issues that arise around the site of the dental implant should be examined and addressed without delay.
We want your dental implant(s) to last your lifetime and bring you as much eating and laughing pleasure as they are known to give. The best way to ensure the success of a dental implant is to follow the aftercare advice your periodontist and dentist provide.
As with a person’s natural teeth, an implant and the tissues surrounding it require regular cleaning. Daily flossing in the area at least once per day is needed after the gums have healed. Some patients prefer interdental brushes to access areas that are more difficult to reach.
 Regular dental check-ups and appointments for cleanings should occur at least twice a year to ensure the longterm success of your implants. Once a quarter may be advised for some individuals who have higher risks for plaque development.
Regular dental check-ups and appointments for cleanings should occur at least twice a year to ensure the longterm success of your implants. Once a quarter may be advised for some individuals who have higher risks for plaque development.
Optimal comfort for our Western Carolina patients has always been a priority. For many, a desired level of comfort and relaxation includes sedation options. Here, we offer several sedation options, including oral and IV sedation (“twilight sleep”). These are administered safely by an anesthesiologist who uses advanced safety equipment throughout your treatment.
If you are considering dental implants, you may wish to begin with a consultation appointment. During this time, we can explain the vast difference in comfort, treatment time, and success available through our specialized skills and extensive technology.
Call 828-274-9440 to schedule. New patients are always welcome.
Mental Health Can Adversely Affect Oral Health
Posted on Mar 06, 2023 by William J. Claiborne, DDS MS
It seems almost every week that I read findings of recent studies that correlate oral health to overall health. It is not surprising that research newly shared reveals connections of how mental health can affect oral health, and vice versa.
It shows that people with mental conditions can be a contributing factor to poor oral hygiene. These conditions include depression, mood disorders, anxiety, OCD (obsessive-compulsive disorders), mood disorders, and eating disorders. These individuals are 2.7 times more likely to experience tooth loss early.
One factor is anxiety and panic, which are often associated with dental treatment.
According to the National Institute of Mental Health, mental illnesses in the U.S. Nearly 1 in 5 adults have with a mental illness (52.9 million in 2020). These numbers have increased post-pandemic.
The Mayo Clinic shared:
“Surveys show a major increase in the number of U.S. adults who report symptoms of stress, anxiety, depression and insomnia during the pandemic, compared with surveys before the pandemic. Some people have increased their use of alcohol or drugs, thinking that can help them cope with their fears about the pandemic. In reality, using these substances can worsen anxiety and depression.”
Poor dental health can be seen in depressed people by a dentist. For example, over 46% of depressed people report tooth pain without apparent cause, known as atypical odontalgia. Too, burning mouth syndrome is an oral condition more common with adults suffering from depression.
Additionally, mental conditions have been linked to oral conditions, such as:
Gum inflammation
Periodontal disease
Cavities
Dry mouth
Chronic jaw and facial pain
Oral ulcers
The relationship between the two – oral health and mental health – seems to lie in cortisol levels. Cortisol is a stress hormone. Stress and anxiety cortisol levels that are too high adversely affect the immune system. This increases the risk of gum disease, oral sores, and infections.
Seeking professional help at the right time is essential to manage an excellent oral and mental state and overall health.
There is also a domino effect once depression or anxiety trigger an imbalance in cortisol. When one’s smile is in poor condition (cavities, stained teeth, missing teeth, bad breath), it can lead to low self-esteem and social isolation. This contributes to a lower quality of life and, in turn, disrupted mental health.
Mental health status has been shown to activate, aggravate or worsen oral problems. These include…
•Gum health and periodontitis (advanced gum disease)
When stress and periodontal disease negatively impact the body’s immune system, inflammation often worsens gum disease. Too, people who endure ongoing stress are more likely to smoke, drink alcohol, or take drugs. These can cause people to neglect maintaining good oral hygiene and be less committed to having regular dental checkups.
•Dry mouth
Eating disorders (such as anorexia nervosa and bulimia) can reduce the amount of saliva – the mouth’s bacteria-rinsing agent. A dry mouth enables the growth of bacteria. Add to this is how many antidepressant medications have a side effect of causing oral dryness.
•Pain in jaw joints
Chronic stress and anxiety are frequent contributors to facial and jaw pain. Teeth grinding and clenching are not uncommon among people with mental conditions. These actions can cause broken, worn or chipped teeth in addition to the painful conditions associated with TMJ disorders.
•Oral ulcers
Lip, tongue, and ulcers inside the mouth can occur more often in people under frequent or chronic stress.
•Developing Cavities
Individuals with mental illnesses are more likely to have dental decay due to a rise in cavity-causing bacterium with a reduced saliva flow – a recipe for developing cavities.
•Tooth erosion
Bulimia is an eating disorder in which vomiting is used to lose weight. Over a third of bulimia patients with eating disorders suffer from tooth erosion due to regurgitated stomach acids that cause tooth erosion.
•Oral cancer
When dental health neglect is coupled with heavy consumptions of alcohol and smoking, the risk of oral cancers increases. Persons who are heavy smokers and drinkers are 50 times more likely to get oral cancer compared to those who never smoke or drink heavily.
Obviously, mental health is closely connected to your oral health. Begin by speaking with a therapist or mental health specialist. Taking care of your mental health is vital to overcome related dental issues.
If you are noticing any of the signs of oral health problems, you should see a periodontal specialist as soon as possible. These signs and symptoms include:
– Bleeding gums when brushing
– Frequent bad breath
– Red, swollen gums
– Gums that are tender or sore
– Gums that pull away from the base of teeth
– Loose teeth
A periodontist is a dental specialist who can help you restore your oral health and enjoy a confident smile. If you’ve experience tooth loss, a periodontist also specializes in the placement of dental implants.
Our Asheville periodontal office also provides sedation options. These include oral and I.V. sedation (“twilight sleep”). These are administered safely by a doctor of anesthesiology who uses advanced safety equipment to monitor you throughout your procedure.
Call 828-274-9440 to schedule an exam or an initial consultation to get to know us better.
Sources include:
https://health.uconn.edu/sbirtacademy/wp-content/uploads/sites/101/2016/08/Dental-brochure.pdf
Simple Ways To Keep A Healthy Smile Throughout The Coming Year
Posted on Dec 27, 2022 by William J. Claiborne, DDS MS
With a new year just ahead, I wanted to remind the smiles in our beautiful Western NC area about ways to have and keep a healthy one!

Nearly every problem that begins in the mouth is due to bacterial overload. Our mouths are constantly being supplied with sustenance for these organisms. Bacteria are able to thrive through the food that enters, especially sugars, and other bacteria-laden items put into the mouth. As bacteria thrive, they are able to reproduce very rapidly.
Insufficient care can lead to a build-up of bacteria, known as plaque. Plaque is a sticky film that forms on teeth when oral bacteria are not removed on a regular basis. In just 48 hours, plaque can harden into a mass that attaches to the base of teeth.
This hardened form of bacteria is known as tartar or calculus. Unlike plaque, tartar cannot be brushed or flossed away. And, once formed, it will continue to amass further.
As oral bacteria reproduce and accumulate, tooth enamel is attacked. The tight seal of gum tissues that surround the base of teeth become inflamed and loosen. This allows for the penetration of running-wild bacteria beneath the gum line. Once this infectious bacteria reaches this point, dental treatment (often ‘planing and root scaling’) is necessary to halt its continued development and restore healthy gums.
If untreated, the stages of gum disease worsen. Eventually, the infectious bacteria of gum disease are able to enter the bloodstream through weakened oral tissues.
Periodontal (gum) disease symptoms include sore gums that bleed when brushing, frequent bad breath, gums that pull away from the base around teeth, and gums that darken in color. As it worsens, pus pockets may form on the gums at the base of some teeth. In advanced stages, gum disease causes teeth to loosen and eventually require removal.
Gum disease often progresses because people are unaware that bleeding or receding gums is actually a symptom. Insufficient brushing, failing to floss and not having regular dental cleanings form a path that begin the process.
Gum disease is an inflammation that attacks teeth, oral tissues and the bone structures that support tooth roots. As the gums pull away from the teeth, darker portions of the tooth are exposed. These are tooth roots sections, now exposed without the protective layer of gum tissue over these areas, leaving teeth vulnerable to bacterial attack.
While the darkersegments of teeth detract from the appearance of a smile, they are also highly sensitive. Drinking hot coffee, eating ice cream or brushing across these areas can send a quick jolt of pain. In addition to periodontal disease, common causes for gum recession can include: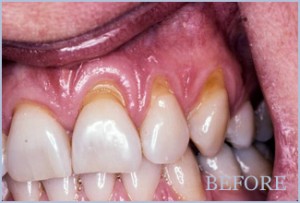
• Rigorous tooth brushing: Using a tooth brush with hard bristles or being too zealous when brushing can wear down enamel as well as gum tissue. Also, abrasive substances such as baking soda are too gritty for teeth and can wear down gum tissues.
• Smoking: A dry mouth is when saliva flow is insufficient to effectively wash bacteria from the mouth. The chemicals in tobacco are terribly drying to oral tissues, which creates an ideal environment for the formation of plaque. Plaque is a build up of oral bacteria that destroys gum tissue and contributes to recession.
• Grinding & clenching teeth: When you clench or grind your teeth during sleep, the force that is placed on teeth can be so strong that they begin to tilt out of position. As this continues, the gums eventually pull away from teeth.
• Hormonal changes: Pregnancy, menopause and puberty can cause changes in hormone levels. These hormonal fluctuations can cause gums to feel tender and be more vulnerable to recession.
• Misaligned teeth: When not properly aligned, teeth endure added force to bite and chew. This can also place added strain to the TMJ (jaw joints), gums and bone that supports tooth roots. This can lead to gum recession.
To avoid the expense and treatment time of gum disease, commit now to thorough oral hygiene and regular dental check-ups and cleanings. Your at-home oral hygiene regimen should include:
– Twice daily brushing with a soft bristle tooth brush and use a fluoridated tooth paste. Brush for at least two minutes each time. Floss daily. Be sure not to pop the floss between teeth to avoid damaging tender gums. Move the floss in a back-&-forth motion between teeth to ease it down so you can scrape the sides of each tooth.
– Use a tongue scrapper daily or brush your tongue with your tooth brush at the end of each brushing. This helps to dislodge bacteria that is embedded in the grooves of the tongue.
– Keep the mouth moist by drinking plenty of water during the day. This will help keep saliva flow at ample levels. Saliva is designed to move oral bacteria from the mouth on a consistent basis. Avoid foods and beverages that are drying to oral tissues such as caffeine, alcohol, and spicy foods. Also, try to minimize the amount of sugar and carbohydrates you consume. These foods amplify the reproduction of oral bacteria.
– Smokers should consider using an oral rinse that replenishes moisture in the mouth. The chemicals in cigarette smoke are very drying to oral tissues. Some oral rinses are specifically designed to replenish oral moisture.
A periodontist is a dentist who has specialized skills in the diagnosis and treatment of all levels of periodontal disease. This specialist can also recontour the shape of gums and place dental implants for optimal results.
In our Asheville periodontal dental office, we feature some of the most advanced technology in dentistry, much of which is not available in other dental offices elsewhere in the Western Carolina region. These features are designed to help maximize comfort, shorten treatment time, speed healing and pinpoint areas of need for the most conservative treatment possible.
If you have not seen a dentist on a regular basis, you may be experiencing symptoms that indicate gum disease. As you would respond to a warning sign with your overall health, so should you with your oral health.
Begin with a thorough periodontal examination to determine what your needs are and the best way to achieve and maintain good oral health. You’ll be supporting your overall health in addition to having a confident smile.
If dental fear or anxiety have prevented you from regular dental care, ask about sedation options. We offer both oral sedation and IV sedation (twilight sleep). Both are safely administered and you are closely monitored by medical personnel who use advanced safety equipment throughout treatment.
Call 828-274-9440 for more information or to schedule an exam appointment.
Recent Posts
Categories
Archives
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- August 2014
- July 2014
- June 2014
- May 2014
- April 2014
- March 2014
- February 2014
- January 2014
- December 2013
- November 2013
- October 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- April 2013
- March 2013
- February 2013
- January 2013
- December 2012
- November 2012
- October 2012
- September 2012
- August 2012
- July 2012
- June 2012


