Header logo
header top contact widget
Blog Archives
Recent Posts
Categories
Archives
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- August 2014
- July 2014
- June 2014
- May 2014
- April 2014
- March 2014
- February 2014
- January 2014
- December 2013
- November 2013
- October 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- April 2013
- March 2013
- February 2013
- January 2013
- December 2012
- November 2012
- October 2012
- September 2012
- August 2012
- July 2012
- June 2012
How NOT To Be The One With Bad Breath!
Posted on Apr 25, 2018 by William J. Claiborne, DDS MS
If you’ve ever wondered “Is my breath bad?” when in close conversations, you know it’s an uneasy feeling. We ALL know this because, when the shoe is on the other foot, being with someone who’s breath odor causes an uncomfortable wall of P-U tends to create a poor and lasting impression!
We all suffer occasionally with not-so-pleasant breath, such as after morning coffee or an onion-topped hot dog lunch. While any bad breath is unwelcome, it is not unusual on occasion. We can often pop a couple of breath mints or piece of gum in our mouths and feel we are somewhat in better shape.
However, it’s when people have frequent bad breath that concerns me, as a dentist, the most.
The root source of bad breath is oral bacteria. Bacteria are living organisms that eat, reproduce and emit waste on a consistent basis. Drinking sugary colas and a diet of high carbohydrate foods rev up bacteria reproduction even more, boosting their ability to grow and thrive.
Poor oral hygiene is the most common cause for bad breath. Not brushing and flossing adequately allows oral bacteria to reproduce, which leads to plaque.
Plaque is the sticky film you feel on teeth when you’ve missed brushing. When not removed daily, plaque forms into a cement-hard substance known to as calculus. This mass is actually a colony of oral bacteria that attaches to teeth and can no longer be brushed or flossed away.
Calculus attacks enamel and gum tissues. As the bacteria grows, it causes the gum tissues to become inflamed. This inflammation can quickly develop into gingivitis, an early form of gum disease. If not resolved fully, however, gingivitis can lead to full-blown periodontal (gum) disease.
Many people are not aware that a common symptom of gum disease is persistent bad breath. This may be accompanied by tender gums that bleed easily when brushing. As it progresses, the gums may loosen from teeth (or ‘recede’) and turn red in color.
When we perform periodontal exams, we look for signs of inflammation and redness. If signs of gum disease are present, we will recommend appropriate treatment to restore your mouth to a healthy state.
While we only recommend the most conservative treatment needed for the level of gum disease that exists, we urge prompt treatment. Gum disease only worsens without treatment and, as with anything, the sooner the problem is resolved, the less involved the process will be. Early treatment can also mean less treatment time and expense.
If gum disease is not the cause of your breath odor, another culprit may be ‘dry mouth.’ Dry mouth causes your mouth to be stale and sticky, which creates bad breath. Dry mouth can be the result of many sources. For example, it is a common side effect of many medications.
Another example of dry mouth is when you first wake up because saliva flow is minimized during sleep. For people who breath through their mouths or snore, this dries oral tissues even more. Unfortunately, this means oral bacteria are not being flushed from of our mouths and able to accumulate.
Other drying causes come from what we may eat or drink. For example, alcoholic beverages, coffee and chocolate are drying to oral tissues. For those who smoke, oral dryness is a particular challenge. Cigarette smoke contains a large number of chemicals that are severely drying.
Want to keep your breath fresh? Preventing bad breath is actually easy. It simply requires a commitment to manage bacteria levels in the mouth.
Begin with a periodontal examination and cleaning to establish a foundation of good oral health. Once your oral health is in good shape, you can keep it there through a thorough daily oral hygiene regimen, which includes:
– Brush at least twice a day for at least two minutes each time. Finish by brushing your tongue with your tooth brush to loosen embedded bacteria there. Be sure to get to the back portion of the tongue, where the majority of oral bacteria are embedded.
– Floss daily to dislodge particles caught between teeth that a toothbrush may not be able to dislodge. If you find this action difficult, consider purchasing an electronic flosser.
– Keep your mouth moist by drinking plenty of filtered water throughout the day. If you take medications that are dying, consider using an oral rinse to boost saliva flow and replenish oral moisture.
Having good oral health and ways is important to having fresh breath. Yet, it is also important to having good overall health. Call 828-274-9440 for more information or to schedule an appointment.
Flossing – Why You Should
Posted on Apr 15, 2018 by William J. Claiborne, DDS MS
If you could do something that required two minutes or less a day, knowing it could save you hundreds or even thousands of dollars a year, you’d do it – right? Then, why is daily flossing such a dilemma for so many people?
According to the American Dental Association (ADA), only 20 percent of American adults floss on a daily basis. (https://www.ada.org/en/publications/ada-news/2014-archive/october/survey-finds-shortcomings-in-oral-health-habits)
As a periodontal specialist with advanced training in the treatment of gum disease, I know the destructive nature of infectious oral bacteria. When an overload of bacteria accumulate in the mouth, cavities form and the gums become food for bacteria.
While many people assume that brushing twice a day is sufficient for maintaining good oral health, brushing often fails to remove food particles that are caught between teeth. These particles begin to rot rather quickly, leaving even more sustenance for bacterial growth and reproduction.
When oral bacteria amass past the point that is manageable by the immune system, the bacteria become infectious. This causes inflammation in the gum tissues, which can eventually lead to the formation of periodontal (gum) disease.
So, if the 1-2 minutes a day required for the act of flossing teeth would prevent cavities and gum disease, then why don’t more people do it? Well, first of all, flossing is not something anyone particularly enjoys. But, like some other basic hygiene tasks, it’s well worth the time and energy – perhaps more than you realize.
The inflammatory effects of the oral bacteria of gum disease don’t just remain in the mouth. Through tears in diseased gum tissues, they are able to enter the bloodstream. As the bacteria travel throughout the body, their toxic nature can trigger inflammatory effects elsewhere.
It is this action that has been the focus of a numerous amount of research over the years. Studies have found that oral bacteria of gum disease are linked to serious health problems. These include heart disease, stroke, preterm babies, arthritis, diabetes, some cancers, Alzheimers disease, erectile dysfunction (ED) and impotency. As research continues, more serious, and even deadly, connections are being made.
Oral bacteria accumulation creates a sticky film in the mouth that is known as plaque. When not removed thoroughly and frequently, plaque can form cement-hard bacteria colonies that attach to teeth. This hardened form of bacteria is known as tartar (or calculus) and, once formed, can no longer be brushed or flossed away.
They key is to keep oral bacteria levels to a minimum, which is why brushing and flossing are an important part of your daily care routine. Yet, as a dental specialist, I understand why it is difficult for some people to develop the habit of daily flossing.
For some, the tight floss around fingers is uncomfortable. For others who have large fingers or problems with manual dexterity, the act of flossing is rather challenging. Yet, for those who floss on a daily basis, it becomes a simple maneuver that is as simple as brushing teeth.
I’ve carefully followed studies that claim flossing provides little benefit. These studies have been under debate within the dental profession due to what some deem as flawed protocols. For example, study participants not being followed long enough to determine true effectiveness or the failure to monitor proper flossing techniques.
What is not, and has never been, debatable, however, is how the action helps to keep oral bacteria levels to a minimum.
As a periodontist, I have a unique view of what the mouth deals with on a day to day basis. If you flossed your teeth, for example, and put the floss under a microscope, you’d likely floss several times a day! Oral bacteria are menacing critters that are destructive in nature – not a pretty sight.
Relook at the advantages you can enjoy as a result of this minutes-per-day action and commit to performing it for a minimum of 2 weeks. You may want to begin by watching a brief video by Colgate on proper flossing techniques at: https://www.colgate.com/en-us/oral-health/basics/brushing-and-flossing/how-to-floss
Our hygienists are also available to assist you personally. They will be happy to help you find a technique that is comfortable and effective. Call 828-274-9440 to begin by scheduling an examination appointment.
Are You ‘Sick’ Of Your Denture?
Posted on Apr 10, 2018 by William J. Claiborne, DDS MS
We often hear people, at times of frustration, exclaim “I’m sick to death of…” or “I’m sick and tired of…”
I think we all have make this claim at one time or another. However, when it comes to wearing dentures or partials, being “sick” of them can go in several different directions. They can, indeed, make you “sick and tired” as well as just plain “sick.”
In 2012, NBC News reported on a study that was published in the Journal of The American Dental Association. The study was conducted to determine methods to effectively kill the bacteria crawling all over the material that make up the gum base of dentures and partials.
What was shocking to many was just how serious the bacteria levels were. Dentures, because of their porous nature, can be coated with a sticky bacteria known as biofilm. It has been found that this biofilm can harbor MRSA or bacteria that is resistant to antibiotics. (https://www.nbcnews.com/healthmain/dirty-dentures-dangerous-mrsa-may-be-lurking-dentists-say-662637)
It was also found that the bacteria in the biofilm doesn’t just stay in the mouth. It can be breathed into the lungs where infections become much more difficult to treat.
Especially concerning is the high number of denture and partial wearers who sleep in their appliances. One study found that wearing dentures while sleeping doubles the risk of pneumonia in elderly adults. (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4541085/)
Remember, bacteria are living, eating organisms. Like any living thing, what eats produces waste. When it comes to oral bacteria, this means that these creatures are defecating in your mouth. That, in itself, is a pretty alarming reality of wearing dentures.
The tiny hide-outs of denture ‘pores’ give oral bacteria an ideal environment to thrive and reproduce. While sleeping in dentures obviously increases the opportunities for this to occur, these icky organisms can create quite an obstacle to adults who have immune systems that are already compromised.
Yet, being “sick” from dentures doesn’t stop there. For those who have worn dentures for many years, the bone that lies underneath the denture has likely shrunk. This process, known as ‘resportion,’ occurs when tooth roots are no longer present in the bone to provide stimulation.
Most denture wearers can sense that something has changed when their once-snug denture begins to slip when eating. Eventually, these slips can cause uncomfortable rubbing on tender gum tissues. The solution, for many, is to alter the diet to include foods that are soft and dissolve easily in the mouth.
The problem with these foods, typically, is they are lacking in the fiber and nutrition necessary for having good overall health. It is no wonder that denture wearers have more gastrointestinal problems and take more medications than people who have their natural teeth.
The problems of dentures go on and on. Renowned implant dentist, lecturer and founder of the Misch Implant Institute, Carl Misch, gives a straight-forward breakdown of the problems associated with wearing dentures in his book, “Dental Implant Prosthetics”
With all the frustrations and complications of wearing dentures, it’s to no surprise that dental implants have become the preferred choice of today’s adult when it comes to replacing natural teeth.
Dental implants are held by the jaw bone, restoring a sturdy foundation for biting and chewing. They also recreate stimulation to the bone that supports them, thus halting the rate of bone loss that occurs from wearing dentures. And, dental implants are designed to last a lifetime, making them an excellent investment.
As a Periodontist, my specialty includes advanced training in the diagnosis and placement of dental implants. Over the years, I have been impressed with their track record, having one of the highest of all implant-in-bone success rates.
Why worry over the health risks associated with wearing dentures and partials? Dental implants are dependable, safe, lasting, and provide a natural look and feel. Call 828-274-9440 to schedule an appointment to determine if dental implants are right for you.
How Dental Implants Can Prevent A ‘Melting Face.’
Posted on Apr 02, 2018 by William J. Claiborne, DDS MS
The aging process isn’t necessarily kind to our appearance. Hair color and texture changes. Age spots creep up. Hair grows where it didn’t used to or thins out in unwanted spots. The skin wrinkles and sags.
While aging gracefully is something we should strive for, it doesn’t mean we’re necessarily thrilled with these changes. Eating a healthy diet and staying active is certainly a good way to stay in shape and retain a more youthful ‘zest’ for life.
While that can help to keep some of the years at bay, some changes caused by the aging process can be avoided, such as wearing sunscreen to avoid age spots. Others can be avoided or halted, including a ‘melting face.’ What is a melting face?
This describes changes to facial appearance when the bone structures that give our face its shape start to shrink. This is caused by the absence of tooth roots from the jaw bone. The stimulation normally provided to the jaw bone from tooth roots no longer exists when natural teeth are removed. This causes the bone to shrink, or ‘resorb.’
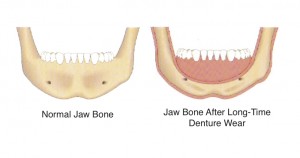
Healthy Jaw Bone Vs Bone Loss From Missing Teeth
As the bone mass declines in height and thins out, changes in facial appearance slowly evolve. For example, as the jaw bone thins, deep wrinkles form around the mouth. Eventually, the corners of the mouth will turn down even in a smile. Jowls form on each side of the face as facial muscles detach from the shrinking bone structure.
As the jaw bone continues to shrink, the chin becomes more pointed and the nose seems to get closer to it. This leads to a collapsed mouth that is known as a ‘granny look.’ This look ages the appearance of an individual far beyond their actual years.
Among the many benefits of dental implants, they also provide stimulation to the jaw bone. This helps to halt the process of bone loss. For those who have already lost a great deal of bone loss, bone rebuilding procedures can be performed to restore a healthy, more youthful face shape.
As a periodontist, my dental specialty includes the diagnosis and placement of dental implants. Dental implants are the closest thing to natural teeth, in many ways.
Dental implants restore the ability to bite and chew comfortably and without worry. Because implants are placed in the jaw bone, this provides the same dependable foundation as you once enjoyed with natural teeth.
Unlike a denture, partial or crown-&-bridge combination, dental implants recreate the stimulation to the jaw bone it needs in order to maintain a healthy mass. People are often surprised to learn that the pressure from wearing a denture or partial actually contributes to the rate of bone loss. For those who sleep in their denture, the accelerates the pace even further.
Some things about the aging process are pretty hard to prevent. Others are totally preventable. With the help of dental implants, the shape of your face and the strength of your jaw bone can be preserved even after tooth loss.
Call 828-274-9440 to schedule a consultation to discuss the dental implant system that is best for your needs as well as the process.


