Header logo
header top contact widget
Oral Cancer
Gum Disease, Tooth Loss Warnings For Smokers
Posted on Jan 29, 2024 by William J. Claiborne, DDS MS
We’re a month in to the new year. If you made the resolution to quit smoking, you may be struggling at this point. But keep up the effort. In addition to the many problems associated with smoking, your smile is also at risk.
As a periodontist in Asheville, NC, I’ve seen how significantly the habit of cigarette smoking can have on one’s smile. It’s no secret that smoking cigarettes can stain teeth and cause bad breath. However, nicotine in any form is a hazardous force in the mouth.
In studies, smokers were 3 – 6 times more likely to have gum disease than nonsmokers. One reason is because smoking is very drying to oral tissues and decreases saliva production. Less saliva means there is less of a natural ‘rinsing’ away of bacteria in the mouth. This leads to higher concentrations of oral bacteria.
Dry tissues also slows healing in the mouth. The longer it takes for tissues to heal, the greater the potential for bacterial complications.
In one study, it was found that smokers were twice as likely as non-smokers to lose teeth in the five years after completing treatment for gum disease. Smokers are also shown to respond less favorably to oral surgery treatments due to slowed healing. For the same reason, dental implants are more likely to fail in smokers.
Researchers who have studied the effects of tobacco smoke on oral tissues say it appears to interfere with the body’s natural ability to fight disease and promote healing. Apparently, smoking affects the way gum tissue responds to all types of treatment, possibly due to tobacco chemicals that interfere with blood flow to the gums. This slows the healing process and makes treatment results less favorable.
According to a study at Temple University, pipe and cigar smokers and users of smokeless tobacco (“chew”) are just as prone to implant complications than cigarette smokers. The study showed three times the amount of moderate to severe gum disease as that of non-smokers.
The American Dental Association (ADA) also warns that smoking can cause the gums to recede from teeth, exposing vulnerable tooth root sections. This enables easier entry of oral bacteria into the structures that support tooth roots. Smoking can also delay healing following periodontal therapy, extractions or implant placement. The longer it takes oral tissues to heal, the greater the risks for infection to develop.
Additionally, smoking increases the risks of oral cancer, lesions inside the mouth, periodontal (gum) disease, enamel erosion and tooth loss. It greatly reduces saliva flow in the mouth, which is a tremendous aid in removing bacteria and food particles from the mouth, helping to control bacteria levels. The condition of “dry mouth” also causes bad breath.
According to the Centers for Disease Control & Prevention (CDC), a smoker has twice the risk for gum disease compared with that of a nonsmoker. (https://www.cdc.gov/tobacco/campaign/tips/diseases/periodontal-gum-disease.html)
When a patient is diagnosed with advanced periodontal disease (periodontitis), they must make a commitment of time and expense to rid this inflammatory disease from their mouths. For those who ignore its presence or assume it will get better on its own, the disease will simply progress further.
Gum disease begins with sore gums that may bleed while brushing teeth. Or, it may cause no noticeable symptoms at all in early stages.
As it worsens, gum disease will cause frequent bad breath, tender gums that turn red, gum recession, and gums that bleed easily when brushing. Pus pockets may form on the gums. As it attacks the structures beneath the gum line, teeth may loosen or shift.
As the nation’s leading cause of adult tooth loss, it brings the hard decisions (and expense) for replacement. After all, you need teeth for eating and speaking. Do you go with dental implants? Or, do you take on the challenges that come with dentures and partials? As hard as the decisions of replacing teeth can be, gum disease can bring even more devastation with it.
Research has linked the bacteria of gum disease to serious health problems. These include heart disease, stroke, preterm babies, arthritis, diabetes, impotency, some cancers and even Alzheimer’s disease. These connections occur through the infectious bacteria of gum disease entering the bloodstream through tears in diseased gum tissues.According to the Centers for Disease Control & Prevention (CDC), a smoker has twice the risk for gum disease compared with that of a nonsmoker.
(https://www.cdc.gov/tobacco/campaign/tips/diseases/periodontal-gum-disease.html)
When a patient is diagnosed with advanced periodontal disease (periodontitis), they must make a commitment of time and expense to rid this inflammatory disease from their mouths. For those who ignore its presence or assume it will get better on its own, the disease will simply progress further.
Gum disease begins with sore gums that may bleed while brushing teeth. Or, it may cause no noticeable symptoms at all in early stages.
As it worsens, gum disease will cause frequent bad breath, tender gums that turn red, gum recession, and gums that bleed easily when brushing. Pus pockets may form on the gums. As it attacks the structures beneath the gum line, teeth may loosen or shift.
As the nation’s leading cause of adult tooth loss, it brings the hard decisions (and expense) for replacement. After all, you need teeth for eating and speaking. Do you go with dental implants? Or, do you take on the challenges that come with dentures and partials? As hard as the decisions of replacing teeth can be, gum disease can bring even more devastation with it.
Research has linked the bacteria of gum disease to serious health problems. These include heart disease, stroke, preterm babies, arthritis, diabetes, impotency, some cancers and even Alzheimer’s disease. These connections occur through the infectious bacteria of gum disease entering the bloodstream through tears in diseased gum tissues.
If you feel your smile is safe by switching to vaping (use of e-cigarettes), read on.
Because of the vape’s moist presence in the mouth, the assumption with vaping over smoking cigarettes is the “benefit” of oral dryness. However, this is easily dispelled when looking at the true facts.

While there are more than 7,000 chemicals found in the smoke of tobacco products, (including nicotine, tar, carbon monoxide, acetaldehyde and N-nitrosamines), nicotine is the primary addicting component. A study of some e-cigarette products found the vapor contains known carcinogens and toxic chemicals, as well as potentially toxic metal particles from the device itself.
The e-liquids delivered by these devices typically contain nicotine, propylene or polyethylene glycol, glycerin, and additives.
In addition to the treatment of all stages of periodontal disease, a periodontist is highly skilled in dental implant placement. Dental implants have become a leading choice in tooth replacement for many reasons, including:
• Dental implants restore one’s natural ability to bite and chew comfortably.
• Dental implants allow people to eat a healthy diet of foods, chewing thoroughly to support good digestion.
• Dental implants enhance confidence when speaking, laughing and dining in social gatherings.
• Dental implants recreate stimulation to the jaw bone like that of natural tooth roots, which helps to halt bone loss.
• Through the prevention of further bone loss, dental implants contribute to the well-big of neighboring teeth
• Dental implants slow the aging changes to facial appearance by preserving jaw bone mass.
• Dental implants, with properly maintenance, are designed to last a lifetime.
One of the most appealing aspects is the longevity of dental implants. Today’s implants are designed to last a lifetime with up to a 98 percent success rate. This is one of the highest success rates for any implant-in-bone procedure.
However, like anything that’s not a natural part of the body, there is a potential for failure. For smokers, the habit is a significant contributor to implant failure.
Studies have shown that people who smoke have more calculus (also known as tartar) than nonsmokers. Calculus is the cement-like buildup on teeth, which is a concentrated mass of oral bacteria. When gums are weakened by an over-accumulation of bacteria, successful integration of dental implants is compromised.
Having a successful outcome with dental implant treatment is worth the efforts to quit smoking. Within two weeks of quitting, gum health improves. (https://www.cancer.gov/about-cancer/causes-prevention/risk/tobacco/cessation-fact-sheet)
In our Western NC periodontal dental office, we intend for every dental implant we place to provide a successful outcome. However, patients who smoke must understand they have higher risks for complications, and even failure of dental implants. The first step is a thorough evaluation of your gums and the existing bone to support dental implants.
At your initial visit, I’ll answer your questions about the process, anticipated costs, and even sedation options. Call 586-739-2155 for an exam appointment or consultation or tap here to begin.
What Gum Disease Bacteria Does To You That May Surprise You.
Posted on Dec 15, 2023 by William J. Claiborne, DDS MS
As we round the corner of another year, making oral hygiene a priority seems a distant thought in the midst of holiday preparations and activities of the season. But, it should be at all times in our lives, for many reasons.
Over the years, research has continuously shown that the bacteria of periodontal disease can have a number of harmful effects – in the mouth AND elsewhere.
This is because these inflammatory bacteria can enter the bloodstream and travel throughout the body. Studies show that these bacteria can activate or worsen a number of serious health problems.
People easily understand that a mouthful of bacteria can cause bad breath and gums that may be tender and redden in color. This makes sense, since an area with a skin cut can redden and swell if it doesn’t heal properly. Yet, because gum tissues are concealed behind cheeks and lips, it is easier to ignore problems that may be clear that something is wrong if more exposed.
To be clear, bacteria in our bodies is not always a bad thing. For example, certain bacteria in the gut actually enhance the process of digestion and help to keep the digestive system operating efficiently.
However, some bacteria are bad. These ignite when too much bacteria invade the body, causing the immune system to become overburdened. Bacterial overload can leave the body’s natural defense response, white blood cells, unable to conquer the infection. So, when a cut becomes infected, your doctor may prescribe an antibiotic to give the immune system added reinforcements.
And, when bacteria overload occurs in the mouth, an inflammatory reaction begins. This is the beginning of gum disease.
Signs of gum disease include bleeding or sore gums, persistent bad breath, receded gums, and/or gums that are red rather than a healthy pink. These are warning signs since gum disease will only worsen without treatment.
As gum disease progresses, gums begin to pull away from the base of teeth, gums become very tender and bleed easily when brushing, pus pockets form on gums and teeth may shift or loosen.
Unfortunately, gum disease is ignored too often by adults in the U.S. The CDC estimates that over 47% of Americans have some level of gum disease, which is also the leading cause of tooth loss.
A periodontist is a specialist in the treatment of all stages of gum disease and in the placement of dental implants. He or she is the expert who can help to restore a bacteria-burdened “oral cavity” to a healthy state.
In addition to a healthy smile, the health of your gums can impact your overall health. By keeping the bacteria of advanced gum disease, known as periodontitis, you lower your risks of a long list of serious health problems that have been shown connected to gum disease bacteria. These include:
• Heart Disease & Stroke – According to research, having advanced gum disease makes you twice as likely to develop heart disease. This is due to clot-causing proteins that occur from oral bacteria that can clog arteries, including the carotid artery that supplies the brain with blood.
• Dementia & Alzheimer’s disease – Studies have shown that tooth loss from oral bacteria is a risk factor for memory loss and early stage Alzheimer’s disease. Apparently, oral infection cause inflammation triggers that can lead to the destruction of brain cells.
• Cancer – Researchers found that males with gum disease are 54% more likely to develop pancreatic cancer, nearly 50% more likely to develop kidney cancer and 30% more likely to have blood cancers.
• Diabetes – Because people with diabetes are more susceptible to infections, with 95% of whom also have periodontal disease.
• Erectile Dysfunction – Men with periodontal disease are 7 times more likely to have erectile dysfunction (ED).
• Premature Birth – Nearly 13% of U.S. babies are born premature, which can lead to breathing issues and infections. Infection in the mother’s body, which includes infection from periodontal disease, can create inflammatory reactions that are related to premature and low birth weight babies.
• Infertility – Research has found that gum disease can complicate attempts for a female to become pregnant.
• Respiratory Problems – When bloodborne bacteria from gum disease reaches the lungs, people with respiratory problems are at higher risk of pneumonia and acute bronchitis (COPD).
It has been said that the mouth is the gateway to the body. Whether it’s the holidays or vacation time or just a busy schedule, your oral health should be a commitment. It takes just minutes a day to brush your teeth thoroughly (at least 2 minutes each time), twice daily, floss daily and swish after meals.
Drink plenty of water, especially after consuming caffeinated beverages or alcohol (including wine). If you smoke, begin with a periodontal exam and ask our hygienist for at-home care instructions.
Call 828-274-9440 if you have questions about your gums or if you are experiencing any of the above mentioned symptoms of gum disease. Also, visit our website to learn more about our sedation options (including “twilight sleep”) and advanced technology, which often reduces treatment time while enhancing comfort.
Laser Dentistry, Cone Beam Imaging Among Our Advanced Features!
Posted on Nov 15, 2023 by William J. Claiborne, DDS MS
Like your “adult” teeth, your gum tissues are irreplaceable. Without question, they deserve the care and attention that come with keeping them healthy and doing their job.
Gum tissues are designed to protect the structures underneath. These include bones, tooth roots, tendons, and muscles to prevent entry of harmful bacteria. Gums are designed to snugly wrap the base of each tooth to keep bacteria from penetrating sensitive root segments of teeth.
Without this protective seal around teeth, the potential for periodontal (gum) disease greatly increases. And gum disease is at concerningly high levels in the U.S. with an estimated 47% of adults having some level of gum disease.
I believe that this high level of gum disease is largely in part due to Americans not being fully familiar with the symptoms. Some are easily ignored or “brushed off” as normal. This is why it is important to be familiar with the signs and symptoms, which include:
• Red, swollen or tender gums or other pain in your mouth
• Bleeding while brushing, flossing, or when eating certain foods
• Gums that pulling away from the base of teeth, making them appear teeth longer
• Loose or separating teeth
• Pus between your gums and teeth
• Sores in your mouth
• Persistent bad breath
• A change in the way your teeth fit together when biting
• A change in the fit of partial dentures
If you are experiencing any of these symptoms, you are urged to seek care with a periodontal specialist as soon as possible. This disease will only worsen without treatment.
Why should you be concerned about periodontal disease?
Gum disease is the nation’s leading cause of adult tooth loss. Additionally, research has linked the bacteria of periodontitis with serious health problems. These include heart disease, stroke, arthritis, diabetes, some cancers, preterm babies, erectile dysfunction (ED) and high blood pressure. Studies on links to Alzheimer’s disease are showing concerning correlations.
A periodontist is an expert in the treatment of all stages of gum disease, including gingivitis, periodontal disease, and the advanced form of periodontitis.
In addition to having these specific skills, I’d like to share the benefits of some of our amazing technology we make available to our Western NC patients. One with a wide range of benefits to patient care is our Dental Laser.
Nd: YAG Dental Laser: This is a small, hand-held device that eliminates or greatly minimizes bleeding during procedures. It also reduces numbing requirements, removes bacteria and easily uncovers gum tissue where dental implants have been placed.
Additionally, laser dentistry can quickly repair oral ulcers and beautifully re-contours or repairs gum tissue with a precision line. Some specific treatments that are ideal for a dental laser include:
Canker & Cold Sores: The laser is also ideal for rapid healing of canker and cold sores. Laser therapy can halt the progression of canker sores, reducing the pain in a day or so. Otherwise, they can last up to 2 weeks. When it comes to cold sores, they are best treated with our laser when the very first symptom arises. Tingling or burning sensation is the first sign that a cold sore is about to erupt. Although lasers can still treat these lesions in later stages, the treatment is most effective in initial stages. Most patients notice significant improvement in comfort after laser treatment with a much shorter duration.
Gum Disease Treatment: In our office, we also use a dental laser to destroy the bacteria of gum disease. This technology also speeds the process and heightens your comfort, saving you treatment time with faster healing.
Correcting a “Gummy Smile”: This is when a smile shows too much gum tissue above upper teeth when smiling fully. We correct this in a procedure known as crown lengthening. In this, a gingivectomy adjusts the height of gum tissues so the smile has a more even smile line. This may involve the use of a dental laser, which provides a precision line and speeds healing.
Balancing a smile line: A gingivectomy is also advised to rebalance the frame of gum tissues that arch the teeth visible in a smile. When one or two teeth have different heights of gum tissue, the smile has a jumbled look. A dental laser can even out the smile line and enhance the beauty of a smile.
Saving a tooth broken near the gum line: When a tooth breaks at or near the gum line, it often requires removal. In some cases, however, we can save the tooth by exposing enough of the structure to receive a crown. This helps the patient to avoid removal and thereby preserves the supporting jaw bone.
In our Asheville NC periodontal dental office, we feature additional technologies, some of the most advanced in the industry. These include:
LANAP Protocol Using PerioLase MVP-7: This process is designed to efficiently and effectively treat periodontitis (advanced gum disease) through laser technology. Treatment is administered with minimal (or no) discomfort and recovery time is minimal. Amazingly, this technology has also been able to stimulate bone regrowth in damaged areas.
Cone Beam 3D Imaging: These views allow us to see your jaw in 3D dimensions and to be able to view it at varying angles. This enables us to see what used to be hidden from view.
Cone Beam images are often used to assess:
• Dental Implant Positions
• Temporomandibular Joints (TMJ)
• Airway Passages
• Bone Structure Damage or Bone Loss
• Teeth, Tooth Roots and Facial Structures
• Signs Of Infections, Cysts, Or Tumors
CS 3600 Intraoral Scanner: Through this process, our patient no longer have impressions made with bulky, goopy trays held in their mouths. This technology quickly and comfortably scans the mouth’s interior for digital impressions using a small, handheld scanner. It can also reach difficult–to–access areas in the patient’s mouth with improved patient comfort.
Simplant Dental Software for Computerized Dental Implant Placement: This system helps in pre-surgical positioning of dental implants on the computer, using a 3D model of the patient’s jaw. This aids in the selection of the implant type to ensure a precision fit.
Intraoral Camera Technology: This provides outstanding quality of images within the mouth. These images are sent to screen for a clear, crisp view so we can confer with patients on specific treatment needs.
Computer Imaging In Treatment Suites: Treatment suites are equipped with computers for convenient image sharing with patients.
Oral & IV Sedation: We take patient comfort very seriously in our Asheville periodontal dental office. That’s a commitment we make to every patient at every appointment. Here, patient comfort is supported by our sedation options. These include oral and I.V. sedation. Also referred to as “twilight sleep” or “sleep dentistry,” these sedatives are administered by a highly-skilled anesthesiologist who uses advanced safety monitoring equipment throughout the patient’s procedure.
My staff and I also take great pride in providing patients with an environment of respect. Some adults come to us embarrassed by the condition of their oral health or missing teeth. Here, we strive to make patients feel they are in the right hands in the right place.
If tooth loss has occurred, a periodontist also specializes in the selection and placement of all types of dental implants. Dental implants, for many reasons, are the preferred option for tooth replacement.
Call 828-274-9440 to schedule a consultation in our state-of-the-art Asheville periodontal dental office. New patients are always welcome and a referral is not always necessary.
A “Lecture-Free” Look At Cigarettes & Your Smile
Posted on Oct 11, 2023 by William J. Claiborne, DDS MS
In this article, I’m going to address cigarette smoking as it affects oral health. This is not intended to lecture or chastise an adult for making a choice to smoke or those caught up in the addictive grip of nicotine. My goal is to relay factual information regarding oral health for smokers so they can better protect their smiles.
Because I’m a native North Carolinian, I’ll begin by sharing some information on our State, as provided by 2018 stats from the CDC (Centers for Disease Control & Prevention).
In 2018, the percentage of adults in North Carolina who smoked was reported as 17.4% (of every 100 adults). The CDC shared findings of all states, with smoking ranged from nearly 9 of every 100 adults in Utah (9.0%) to 25 of every 100 adults in West Virginia (25.2%).
They also shared that cigarette smoking was lowest among those with a graduate degree (3.2%) and highest for those who had only achieved a GED certificate (30.7%). Those with a high school diploma showed a lower percentage of nearly half of the GED level adults at 17.1%.
As an Asheville periodontal dental specialist, smoking is a particular concern since many people are unaware of the oral health risks. While many smokers are familiar with the risks smoking poses related to cancer and other diseases, smoking is also terribly harmful to your smile.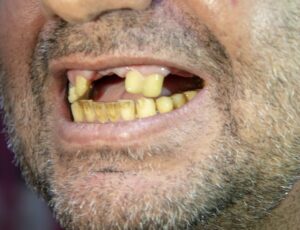
For instance, smokers have a greater risk of periodontal (gum) disease. The drying effect that smoking has on the soft tissues in the mouth offers an ideal breeding ground for oral bacteria. This enables easier entry of oral bacteria into the structures that support tooth roots.
According to the Centers for Disease Control & Prevention (CDC), a smoker has twice the risk for gum disease compared to that of a nonsmoker.
As oral bacteria thrive and reproduce in the mouth, gum tissues become tender and inflamed. These are signs of gingivitis, the beginning stage of gum disease.
Gum disease at this stage can cause persistent bad breath, swollen gums and gums that bleed easily when brushing. As it progresses, gum tissues turn red or purple from inflammation. Pus pockets may form at the base of some teeth. This advanced stage is known as periodontitis.
Eventually, the infectious bacteria penetrate below the gum line and attack supporting bone and the tissues surrounding tooth roots. This can cause teeth to loosen and eventually require removal. Gum disease is the nation’s leading cause of adult tooth loss.
Losing teeth is detrimental to your overall health and not a normal part of the aging process. Studies have shown that people who wear dentures die an average of ten years earlier than those who keep their natural teeth.
Denture wearers also have higher incidences of pneumonia, and worse. A 2015 report by NBC News shared findings surrounding dentures and MRSA biofilm. The report included a dental specialist’s warning that, “Concern about biofilms on dentures is growing as researchers continue to identify links between oral bacteria and heart disease, chronic obstructive pulmonary disease or COPD, and respiratory diseases, including aspiration pneumonia.”
Many smokers are aware that they have stained teeth and more-frequent bad breath than non-smokers. They also have slower healing periods after procedures such as extractions, gum treatment and oral surgery.
Although a hygienist may go slowly and gently, dental cleanings are typically less comfortable for smokers. This is because smoking causes a greater buildup of plaque. With gum tissues already tender from the bacterial irritation of plaque, removing buildup from between and around the base of teeth adds to the discomfort of inflamed tissues.
According to the American Dental Association (ADA), smoking increases the risks of oral cancer, lesions inside the mouth, enamel erosion and tooth loss in addition to periodontal (gum) disease.
If you vape, remember that nicotine in any form is a hazardous force in the mouth. And the vapor itself is not safe for oral health.
Vaping (using e-cigarettes) delivers nicotine through an inhaled mist. Although the vapor is generally not labeled as “dangerous,” one study of some e-cigarette products found the vapor contains known carcinogens and toxic chemicals, including, propylene or polyethylene glycol, glycerin, and additives. And, its nicotine is no less harmful to the user as that delivered via cigarette smoke.
Unfortunately, many cigarette users switch to vaping based on the perception that “e-cigs” are a safer alternative. For those hoping to wean themselves off cigarettes through this switch, very few achieve that goal as a result.
A 2018 report by the National Academy of Sciences, Engineering, and Medicine concluded there was “evidence that e-cigarette use increases the frequency and intensity of cigarette smoking in the future.”
Although the focus in this article is meant to be on oral health, allow me to reiterate some of the benefits of “kicking the habit” …
• Smokers have a decreased life expectancy of an average of 10–15 years compared to non-smokers.
• Smoking is linked to nearly a third of all cancer diseases and deaths.
• Pregnant women who smoke have a higher risk for first-trimester spontaneous abortion, preterm births, low birth weight babies and sudden infant death syndrome (SIDS).
• Women who smoke are at risk for early menopause while men who smoke are more at risk for impotency.
• People who breathe in your “second hand” smoke (what you exhale) are subjected to over 50 known carcinogens and other harmful chemicals.
For those who are able to give up smoking, the effort is well worth it. The positive effects can be felt almost immediately. In about 48 hours, damaged nerve endings begin to restore. The sense of smell and taste begin to return to normal.
“Quitters” also notice their breathing is easier in about 3 days and they have fuller air intake. Oral health improves within 2 weeks as blood circulation in the gums and teeth returns to nearly that of non-smokers. Heart attack risk also declines with blood flow greatly improving. Activities are easier and the constant smokers cough is gone.
 In our Asheville periodontal office, our goal – for every patient – is to help each achieve optimal oral health and a smile he or she is proud to share. For those who smoke, we make individualized recommendations so the potential for achieving this is favorable.
In our Asheville periodontal office, our goal – for every patient – is to help each achieve optimal oral health and a smile he or she is proud to share. For those who smoke, we make individualized recommendations so the potential for achieving this is favorable.
If tooth loss has already occurred, we are specialists in the treatment of all stages of gum disease and in the diagnosis and placement of dental implants. We will be happy to discuss the dental implant system that may be best for your needs.
Or, if dental fear or anxiety have kept you from receiving regular dental care, ask us about oral or IV sedation (“twilight sleep”). These sedatives are delivered by an MD of anesthesia for your optimal safety and comfort. And, in all procedures, we make patient comfort a high priority.
Call 828-274-9440 to schedule an examination.
Sources:
https://www.cdc.gov/tobacco/campaign/tips/diseases/periodontal-gum-disease.html
https://www.sciencedaily.com/releases/2016/11/161116101821.htm
https://www.nbcnews.com/healthmain/dirty-dentures-dangerous-mrsa-may-be-lurking-dentists-say-662637
https://www.cdc.gov/tobacco/basic_information/e-cigarettes/index.htm
Recent Posts
Categories
Archives
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- August 2014
- July 2014
- June 2014
- May 2014
- April 2014
- March 2014
- February 2014
- January 2014
- December 2013
- November 2013
- October 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- April 2013
- March 2013
- February 2013
- January 2013
- December 2012
- November 2012
- October 2012
- September 2012
- August 2012
- July 2012
- June 2012


